Typically, ethnic skin ranges from Types III to VI. These clients have more richly pigmented skin tones and experience unique skin care challenges, such as skin discoloration and changes in skin texture. Some of these conditions are native only to people of color, whereas others might be seen in all groups, but are especially common in people of color.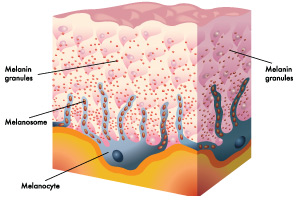
MELANIN
Melanin is a natural, dark pigment produced by melanocytes, which are found in the basal layer of the epidermis. Melanocytes use the amino acid, tyrosine, to produce melanin. Melanin is responsible for adding pigmentation to skin, nails, eyes, and hair. It is also known as an absorber of light. Because of this unique characteristic, the melanin found in the skin aids in protection against UVB radiation and skin cancers. Melanin also plays a protective role against fine lines, wrinkles, and enlarged pores. It is because of this reason that people who are highly pigmented show little signs of skin aging when compared to people of lighter complexions.
HYPERPIGMENTATION
All people are prone to skin discoloration, which occurs secondary to injury to the tissue of the skin. One of the most challenging aspects of ethnic skin care is treating discoloration, specifically hyperpigmentation and hypopigmentation. Skin discoloration can come from using products that contain ingredients that cause irritation or dryness. This discoloration occurs because melanocytes are more reactive, secondary to inflammation, resulting in an increase in melanin production. Clients who have dry, sensitive skin are prone to
skin discoloration.
Injury to the skin includes inflammation, sun damage, trauma, and acne. When a reaction to certain ingredients occurs in Types I and II, the skin will return to its normal state once the use of the offending ingredients is discontinued. In Types III through VI, however, if a reaction occurs, it is usually followed by post-inflammatory hyperpigmentation, which typically develops after one to two weeks of exposure to that ingredient and can last up to several months. Post-inflammatory hyperpigmentation related to acne can take months to years to heal.
Management of hyperpigmentation is dependent on the cause. Treating the underlying offending agent is essential. Removing harsh ingredients and products from the client's skin care regimen can help treat acne and other troubled areas on the skin. Incorporating a broad spectrum sunscreen with an SPF of 30 or higher into the daily regimen will aid in preventing and treating hyperpigmentation. In addition, the client should consider consulting their family doctor or dermatologist for the recommendation of topical treatments, including retinol, alpha hydroxy acid, kojic acid, topical glucocorticoids, hydroquinone, and azelaic acid.
 Melasma
Melasma
Melasma is a less common form of hyperpigmentation that typically appears on the face. It is a darkening skin condition that is commonly found in women who are exposed to the sun for prolonged periods of time. In this condition, estrogen and progesterone stimulate melanocytes to produce more melanin, all as a result of sun exposure. Because it is closely associated with a hormonal imbalance, melasma is seen in women of reproductive age. Another cause of melasma is the intake of oral contraceptives. The dark patches are typically deposited on sun-exposed areas, including the cheeks, chin, and forehead. The discoloration can be so pronounced that it may cause self-image concerns. Although melasma can occur in any race, it is commonly seen in Hispanics and Asians.
Another form of melasma is chloasma, which is seen in pregnancy. This condition presents itself in the same way as melasma. The management of melasma should start with prevention. Clients should use a broad spectrum sunscreen with an SPF of 30 or higher year-round and wear protective clothing, such as hats and long sleeves, when they know that they will be exposed to the sun for a prolonged period of time. Using sunscreen is critical in clearing up symptoms and preventing a recurrence. Sunscreen use is safe during pregnancy, so pregnant women should apply it daily as well. Chloasma typically goes away after giving birth. Both hydroquinone cream and Retin-A cream are approved topical treatments for melasma.
When clients are dealing with hyperpigmentation, it is crucial to inform them to never use skin bleaching products that contain steroids as they can cause permanent skin discoloration.
HYPOPIGMENTATION
Hypopigmentation is the loss of skin color caused by the depletion of melanocytes or tyrosine. It leads to reduced melanin production. Causes of hypopigmentation include the use of chemical skin bleaching products, Imatinib (anti-cancer medication) therapy, laser treatments, and various disease conditions such as albinism, leprosy, vitiligo, tinea versicolor, and pityriasis alba. Though much less common than hyperpigmentation, hypopigmentation can be difficult to treat. One popular approach is to treat the underlying cause by the discontinuation of the offending agent.
Vitiligo
Vitiligo is a condition of depigmentation where only portions of the skin lose their pigment, resulting in pale patches on any part of the body. These patches start out small, but typically grow in size. This growth occurs because the skin pigment cells either die or lose their ability to function. There are several speculated causes of vitiligo, including idiopathic autoimmune processes, genetic susceptibility, viral causes, overall changes in the immune system, environmental factors, chemicals (the result of bleaching the skin), and oxidative stress. Though vitiligo can be diagnosed clinically, true diagnosis involves examination of the skin under ultraviolet light. When skin affected by vitiligo is exposed to ultraviolet light, it illuminates the color blue. When normal skin is exposed to ultraviolet light, there is no illumination or glow.
There is no known permanent treatment for vitiligo, however, some clients choose skin camouflage, phototherapy, immunosuppressants such as topical steroids, calcineurin inhibitors, or depigmentation, a permanent and vigorous process that depigments the unaffected skin. Health professionals treating vitiligo should also focus on the psychological aspect of the disease. Having vitiligo can lead to depression or similar mood disorders. Therefore, it is important to focus on the whole client as opposed to just his or her physical changes. As with all skin conditions, skin protection is important. The daily use of sunscreen with an SPF of 30 or higher is highly recommended. Clients with vitiligo should avoid unnecessary sun exposure of the unaffected skin as it can be hazardous.
SCARRING ALOPECIA
Hair loss is a common aging phenomenon. While scarring alopecia (cicatricial alopecia) is seen in all people, it is most commonly seen in women of African descent. It is caused by inflammation and destruction of the hair follicle, followed by a replacement with scar tissue. The scar tissue formed on the scalp leads to permanent hair loss. There is speculation that this form of alopecia is related to the use of chemical hair treatments, however, this condition is also seen in women who have worn their hair natural all of their lives. Signs and symptoms rapidly progress and include bald spots, scalp itching, inflammation, redness, scaling, dryness, burning, and pigmentation changes. Scarring related to inflammation and follicle destruction is actually below the scalp, so individuals cannot see an actual scar. Diagnosis of scarring alopecia can be made by a skin biopsy or trichoscopy.
The treatment of scarring alopecia is difficult, so it should be left to a dermatologist who specializes in hair and scalp treatments. It is important to note that hair growth cannot be restored once the follicles have been destroyed, therefore, women should look to a specialist to discuss treatment options. The goal of treatment is to reduce the inflammation, thereby reducing the level of scarring. Treatments include oral medications such as antibiotics, steroids, immunosuppressants, and topical modalities such as steroids, calcineurin inhibitors, solutions, and oils. It is appropriate to use gentle shampoos and hair products, as well as wigs, hats, hair pieces, and head wraps. Some clients undergo hair restoration surgery or scalp reduction. Because losing hair can lead to depression and mood disorders, it is important that health professionals treating scarring alopecia take their clients' mood and self-esteem
into consideration.
TEXTURAL CHANGES
There are also texture changes that occur with ethnic skin, including eczema and keloid formation.
Eczema
Eczema is also known as atopic dermatitis and is an inflammation of the skin that results in red, itchy, swollen, scaly, cracked skin and typically presents anywhere on the body. Eczema affects all races, but is commonly seen in people of color. There are several factors causing eczema including genetics, environmental changes, and immune system dysfunction. Factors that may exacerbate symptoms of eczema include emotional stress, excessive hand washing, detergents, harsh ingredients in skin care products, cigarette smoke, dust, chlorine, and wool clothing. A hallmark of eczema is itchiness and the appearance of scaly skin. It is diagnosed by atopy patch testing and its treatment starts with discontinuing or avoiding the offending agent, applying daily moisturizers or emollients to skin, and taking warm baths. Medical treatment includes topical steroids, calcineurin inhibitors, and systemic immunosuppressants. Ultraviolet light therapy has also been effective in reducing the flare-ups of eczema.
Keloids
Keloids also affect all races, but are predominantly seen in people of African descent. A keloid is a type of scar that is an overgrowth of granulation tissue at the site of a healed injury. They are firm, raised, rubbery, and pearly looking scars and are typically darker than the skin and have a smooth texture. One characteristic of the keloid scar is that it grows beyond the initial wound. Keloids derive from pimples, scars, burns, ear piercings, vaccine sites, and surgical scars. Treatment of keloids starts with prevention of injury or trauma to the skin. Medical treatment is age dependent because some medications – including steroids, radiotherapy, and anti-metabolites – are associated with growth abnormalities in children. In adults, treatment of keloids include external beam therapy, kenalog injections, corticosteroids, and cryotherapy.
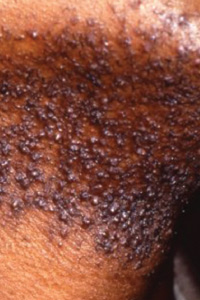 PSEUDOFOLLICULTIS BARBAE
PSEUDOFOLLICULTIS BARBAE
Pseudofolliculitis barbae, also known as razor bumps, is a skin condition that causes textural changes. It is a persistent irritation caused by shaving, is common in men of African descent, and typically appears in parts of the skin that are absent of hair. The mechanism behind the condition has to do with the type of hair. Since people of African descent have naturally curly, coarse, or thick hair, their hair tends to curl into the skin as opposed to coming straight out of the hair follicle. This pattern of growth leads to inflammation and small bumps. If untreated, razor bumps can cause keloid formation. A form of pseudofolliculitis barbae is ingrown hairs. To prevent these razor bumps, men should either let their beard grow or cut their hair to a length of one millimeter so it does not curl back into the skin. Medical treatment options include glycolic acid peels, salicylic acid peels, antibiotic topical gels, and Retin-A cream, which aids in evening out the scarring. Permanent hair removal is the most definitive treatment.
When it comes to managing and treating ethnic skin conditions, one important thing to keep in mind is the skin sensitivity level of clients who are richly pigmented. For example, a client with lighter skin color may benefit from laser treatment or a chemical peel. However, those same treatments may cause scarring, hypopigmentation, or hyperpigmentation with someone of a darker complexion. Various ethnicities are associated with numerous skin conditions. People of Asian descent are prone to hypopigmentation, hyperpigmentation, age spots secondary to sensitivity in melanocytes, and melasma. People of Hispanic descent are prone to post-inflammatory hyperpigmentation from acne scarring, melasma, and irritation from insect bites. People of African descent are prone to post-inflammatory hyperpigmentation from acne scarring, pseudofolliculitis barbae, keloids, and melasma.
Clients with highly pigmented skin are at low risk of developing skin cancer because the epidermal melanin in their skin is higher, thereby protecting them against sun damage. Their risk is much lower than clients with low-pigmented skin. Because of this phenomenon, it is more difficult to detect skin cancers in clients with darker complexions. Therefore, the daily use of SPF 30 or higher is important in the prevention of skin cancer. Consistent SPF use also helps prevent darkening of spots related to post-inflammatory hyperpigmentation. Treating ethnic skin conditions is a rising concern that should not be taken lightly. Regimens should always include a gentle cleanser, moisturizer, and sunscreen.
 Dr. Gina Charles is the founder of Dr. G Makeup Artist, a makeup and skin care company, aimed at enhancing natural beauty and providing non-invasive treatments for various skin conditions. Charles provides a variety of services, including treatment of acne, hyperpigmentation, and bridal makeup. Charles is a family medicine physician, makeup artist, skin care professional, and global philanthropist. Between medically treating people and spear-heading Dr. G Makeup Artist, she volunteers her makeup services for breast cancer survivors, and mentors young women in career development. By combining her love for medicine and beauty, Charles proudly serves women of all ages.
Dr. Gina Charles is the founder of Dr. G Makeup Artist, a makeup and skin care company, aimed at enhancing natural beauty and providing non-invasive treatments for various skin conditions. Charles provides a variety of services, including treatment of acne, hyperpigmentation, and bridal makeup. Charles is a family medicine physician, makeup artist, skin care professional, and global philanthropist. Between medically treating people and spear-heading Dr. G Makeup Artist, she volunteers her makeup services for breast cancer survivors, and mentors young women in career development. By combining her love for medicine and beauty, Charles proudly serves women of all ages.
Want to read more?
Subscribe to one of our monthly plans to continue reading this article.