It is estimated that one American dies every hour from skin cancer.1 Even though the rate of many other common cancers is falling, the incidence of melanoma continues to increase significantly and at a faster rate than any of the seven most common cancers.2 Each year there are more new cases of skin cancer than the combined incidence of breast, prostate, lung, and colon cancers.3
 Skin care professionals are often the first line of defense in evaluating a client’s skin for cancer and recommending further follow up with their physicians. Professionals are also able to clearly visualize parts of the body that the client may not be able to see themselves. It may literally be a matter of life and death for professionals to have a general knowledge of the three most common skin cancers and to actively screen clients for cancer while performing treatments.
Skin care professionals are often the first line of defense in evaluating a client’s skin for cancer and recommending further follow up with their physicians. Professionals are also able to clearly visualize parts of the body that the client may not be able to see themselves. It may literally be a matter of life and death for professionals to have a general knowledge of the three most common skin cancers and to actively screen clients for cancer while performing treatments.
There are three types of skin cancer with which skin care professionals should be well versed and consciously on the lookout: basal cell carcinoma, squamous cell carcinoma, and melanoma.
 Basal Cell Carcinoma
Basal Cell Carcinoma
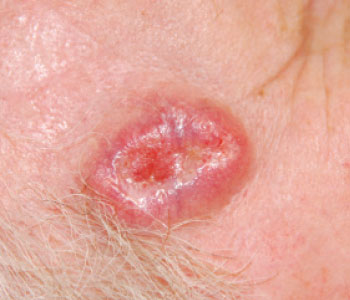
Basal cell carcinoma (BCC) is a cancerous lesion that arise in the skin’s basal cells, cells that line the deepest layer of the epidermis. Anyone who has been exposed to the sun can develop a BCC and those most at risk have fair skin, light hair and light eyes. BCC may look like an open sore, red patch, pink growth, shiny bump, or scar. It may also bleed if scratched. While BCC rarely goes on to metastasize, it may become disfigured if not removed
soon enough.
Squamous Cell Carcinoma
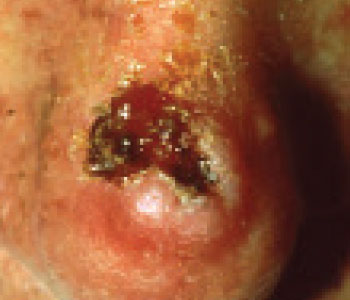
Squamous cell carcinoma (SCC) is three times more common than BCC. SCC is an uncontrolled growth of abnormal squamous cells, which are the cells that compose most of the epidermis. SCC is frequently found on sun-
exposed areas, most commonly the head, neck, ears, lips, back of the hands, and forearms. It often looks like a scaly red patch, open sore, or elevated growth or wart and may crust or bleed. It may also grow rapidly and can become disfigured and sometimes deadly, if allowed to progress.
Melanoma
Melanoma is the most dangerous type of skin cancer and, although it only makes up two percent of all skin cancers, causes 77 percent of skin cancer deaths. It is a neoplasm of the melanin producing cells of the skin and presents most commonly as a brown or black skin lesion with irregularities in symmetry, border, and coloration. The most difficult type of melanoma to diagnose is amelanotic, a type of melanoma that lacks pigment and has a normal skin color. This type of melanoma has an irregular shape and may sometimes present with a faintly-pigmented border. It may also be slightly raised.
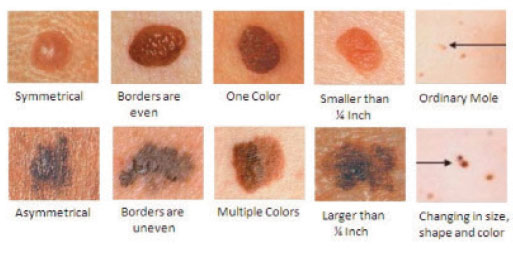
Melanoma may develop within an existing mole or on normal skin. It has a high fatality rate because its cells can break off and metastasize. When attempting to diagnose melanoma, it is beneficial to use the “ABCDE” rule, a convenient mnemonic to run through while screening the client’s skin. If the lesion agrees with one or more of the following descriptions, it is highly suspicious for melanoma:
A: Asymmetry – One-half does not match the other half.
B: Borders – The border of the lesion is irregularly shaped, ragged, notched, or blurred.
C: Color – The pigmentation is not uniform. Mixed shades of tan, black, and brown with dashes of red, white, and blue may add to the lesion’s appearance.
D: Diameter – The width of the lesion is greater than six millimeters, about the size of a pencil eraser. However, any sized lesion with a noticeable amount of growth should be evaluated for cancer.
E: Evolution – The size, color, border, or symmetry of a mole has changed over time.
If a client mentions that they have a sore that does not heal, a mole that has begun to itch or become painful, or has found a new growth, especially on the palms of their hands or the soles of their feet, professionals should be especially concerned about that lesion being skin cancer. Ultimately, it is always a safe bet to simply recommend that a client with any questionable lesion follow up with their primary care doctor or dermatologist for a biopsy to determine if the spot is cancerous or not.
References
1 American Cancer Society. Cancer Facts & Figures 2015.
2 Howlader N, Noone AM, Krapcho M, et al (2009). SEER Cancer Statistics Review.
3 American Cancer Society. Cancer Facts & Figures 2015.
Want to read more?
Subscribe to one of our monthly plans to continue reading this article.