Educating teenagers on the causes of acne, dispelling the myths, and explaining how to best treat acne is a crucial step in providing teenagers that suffer from acne with a sense of empowerment to replace feelings of helplessness.
Causes of Acne
Acne occurs when hair follicles become plugged with oil and dead skin cells. This buildup causes bacteria to breed and the skin to become inflamed. Acne typically appears on the face, neck, chest, back, and shoulders, the areas with the most sebaceous glands.
The main causes of acne include hyperkeratinization, the excessive buildup of skin cells inside the hair follicle; overactive sebaceous glands; multiplication of P.acnes bacteria; and inflammation of the hair follicle and the surrounding tissue.
P.acnes grow on both normal and blemish-prone skin, but are present in abnormally-high numbers of teenagers experiencing breakouts. P.acnes bacterium flourishes in the anaerobic environment created by clogged pores with excess sebum to digest.
Blame the Hormones
It is not clear why some teenagers are more prone to blemishes than others. It is known, however, that androgens play a role. A hormone is a chemical messenger that travels through the bloodstream, stimulates the activity of other organs, and eventually affects cellular functions. Androgens are produced by the ovaries and the adrenal glands in women and by the testes in men. Androgen hormones are responsible for increasing the size and productivity of the sebaceous glands. Androgens increase in both males and females during puberty.
Ingrown Hairs
A teenage male's testosterone levels surge during puberty, resulting in breakouts that are typically more severe than ones that are experienced by a teenage female. Acne peaks for the young male between the ages of 16 and 19 and normally clears by the age of 20. Teenage males can also develop pseudofolliculitis barbae (ingrown hairs) when they begin shaving. While ingrown hairs look like acne lesions, they are actually inflamed hair follicles. The teenager can treat flare-ups with products containing salicylic acid and anti-inflammatory ingredients.
Cyclical Acne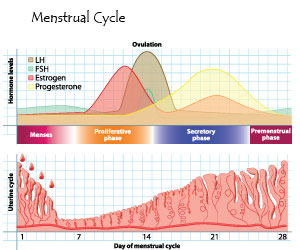
Hormonal changes related to a female's menstrual cycle increase testosterone levels and lead to blemish-prone skin. Breakouts in females peak between the ages of 14 and 17. As a teenage female enters puberty, her body begins producing various hormones that cause the eggs in her ovaries to mature, inducing ovulation.
The hypothalamus releases the follicle stimulating hormone releasing factor (FSH-RF), a chemical messenger, that tells the pituitary gland to secrete follicle stimulating hormone (FSH) and a small amount of luteinizing hormone (LH) into the bloodstream. These hormones cause the follicles holding the eggs within the female's ovaries to begin maturation.
As the follicles ripen over a seven-day period, they secrete more and more estrogen into the bloodstream. When the estrogen level reaches a certain point, it causes the hypothalamus to release luteinizing hormone releasing factor (LH-RF) telling the pituitary gland to release a large amount of LH. The surge of LH triggers the most mature follicle to burst, releasing an egg, on or around day 14 of a 28-day cycle.
The menstrual cycle graph shows that estrogen levels increase during days seven through 12. It also shows that progesterone levels, which are responsible for bloating and the tightening of the pores, begin to increase on or around day 14. Furthermore, as estrogen levels decline, testosterone, which is responsible for oil production, becomes the dominant hormone.
Increasing testosterone and increasing progesterone is a recipe for breakouts! Females usually break out the week before their period, with their skin beginning to clear as menstruation commences. Young women can gain the upper hand on cyclical acne by spot treating the cheeks and jawline with salicylic acid the week prior to menses, cleansing with alpha hydroxy acid cleansers, and considering monthly professional exfoliation the week prior to menstruation.
Additional Contributing Factors to Teenage Acne
Genetics. If a teenager's parents had acne, the teenager is prone to developing it as well.
Medications. Some medications, such as epilepsy medication, prednisone, DHEA, bromides, iodides, and lithium, can cause acne.2
Cosmetics. Certain cosmetics can clog pores. Water-based cosmetics are less likely to cause acne than oil-based products; look for non-comedogenic makeup.
Emotional Stress. Stress exacerbates just about every disease, including acne. Stress causes the body to release cortisol, which contributes to sebum production. Teenagers should look for an effective outlet to deal with stress before it becomes overwhelming.
Lack of Sleep. Adolescents are notorious for not getting enough sleep. Studies from the Bradley Hospital show that most teenagers need nine and a quarter hours of sleep a night but most teenagers only get between seven and seven and a quarter hours of sleep. Teenagers may experience sleep deprivation because a shift in their internal time clock, by about two hours later, occurs at puberty. Furthermore, in order to stay awake during school hours because of the shift, some teenagers turn to highly-caffeinated energy drinks, which exacerbate sleep deprivation.3,4
Teenagers may also experience social and school obligations, including homework, sports, and after-school activities, that lead to over commitment; in order to fulfill their responsibilities, they may cut out on much-needed sleep.
Teenagers often indulge in inappropriate bedtime snacks that raise blood sugar levels and delay sleep, particularly grains and sugars. In the early morning hours when their blood sugar drops too low, they wake up and may be unable to fall back asleep. A change in their bedtime snack may help resolve this issue.
The Environment. Acne can develop whenever the skin comes into contact with oils or grease, such as products that might be found in a work area, like a kitchen with fry vats. Hot, humid environments, like dry cleaning stores, can cause a person to sweat, creating a breeding ground for bacteria. Many teenagers break out more in the humid summer months.
Diet. Studies indicate that certain dietary factors, including dairy products and carbohydrate-rich foods, can trigger acne because they cause the insulin levels within the body to rise. Eating refined carbohydrates and sugar causes a surge of insulin and an insulin-like growth factor (IGF-1) in the body. High levels of insulin and inflammation contribute to the release of cortisol. IGF-1 also causes hyperkeratinization, another cause of acne.
High insulin levels cause a chemical chain of events to take place within the hair follicle. The spike in insulin leads to an excess of androgen hormone production, causing sebaceous glands to secrete sebum. Testosterone is then metabolized by an enzyme known as 5 alpha-reductase and converts to dihydrotestosterone (DHT). As a result, DHT stimulates a receptor at the base of the hair follicle. The stimulated receptor site sends a signal to the sebaceous gland to produce more oil.
The top diet-related acne offenders are sugar and grain carbohydrates because they convert into glucose in the body. Some common foods to avoid are bread, cereal, pasta, rice, potatoes, corn, and foods that are high in starch. Clients should look for foods that are low on the glycemic index to avoid rises in insulin.
Actions that make acne worse by increasing inflammation, oil production, or bacteria include friction, rubbing, harsh scrubbing, stress, and tanning beds. Acne can also worsen due to sun exposure, cleansing too often; picking or squeezing; not using a moisturizer or sunscreen; over applying topicals or overuse of astringents; comedogenic makeup; wax-heavy hair products; and incorrect or ineffective products.
Acne Progression
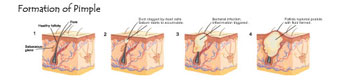
Excessive amounts of keratinocyte cells adhere to the follicle walls while increased sebum is produced; this buildup forms a plug that blocks the pore, creating an open or closed comedone. Sebum production continues as P.acnes bacteria build up and multiply, causing inflammation and creating a papule. The inflammation increases as P.acnes bacteria continue to multiply. As a result, white blood cells accumulate as a part of the immune system response, weakening the hair follicle wall and causing it to rupture; at this stage, a pustule is formed. Nodules and cysts soon begin to form due to the increased inflammation; furthermore, tissue destruction is incurred by the ruptured
follicle wall.
Common Types of Teenage Acne
Hormonal Acne. This type of acne is caused by an increase in androgen hormones that initiate overactive sebaceous activity. Hormonal acne normally appears along the chin and jawline.
Asphyxiated Acne. Asphyxiated acne is characterized by a rough surface and caused by dead cell buildup with oil and debris trapped beneath it. It is very common in
drier climates.
Inflammatory Acne. This type of acne presents as red, inflamed skin and is very uncomfortable; it is best concealed by blending the edges of each lesion with concealer rather than covering up the
whole pimple.
Cyclical Acne. Cyclical acne is the monthly breakout that occurs the week prior to menstruation.
 Acne Cosmetica. This form of acne is caused by comedogenic or irritating products, usually from makeup. The offender may also be laundry or hair care products.
Acne Cosmetica. This form of acne is caused by comedogenic or irritating products, usually from makeup. The offender may also be laundry or hair care products.
Acne Mechanica. Acne mechanica is caused by friction against the skin and may be the result of a football helmet, shoulder pads, or any other object worn next to the skin.
Bacterial Acne. This form of acne occurs due to an overabundance of the P.acnes bacteria.
Nodular or Cystic Acne. Nodular or cystic acne is a very painful form of acne where a large nodule forms under the surface of the skin. The teenager should see a dermatologist if nodules or cysts are developing as they can result in scarring.
Systemic acne. This type of acne appears on the face and on other areas of the body. It is commonly due to medication, diet, or even illness.
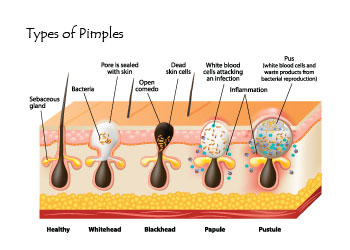
Types of Pimples
There are four types of pimples that are characterized by a number of different factors. A whitehead contains bacteria in the pore and is sealed with skin. Blackheads contain dead skin cells and have open comedones. Papules and pustules are both characterized by inflammation. Papules, however, contain white blood cells that are attacking an infection. Pustules hold pus, which is a combination of white blood cells and waste products from bacterial reproduction.
There are also five grades of acne that commonly affect teenagers. Grade I is characterized by open and closed comedones and is considered mild. This grade consists of whiteheads and blackheads. Grades II and III are characterized by papules and pustules. Grade II is moderate with an increased number of whiteheads, blackheads, and papules. Grade III adds inflammation and pustules. Grade IV consists of nodules and cysts and is considered severe. This grade is characterized by blackheads, whiteheads, papules, pustules, nodules, and cysts. Milia, which is formed by hard keratin cells that are trapped below the surface of the skin, can be present in any grade; it is removed by a lancet.
Common Acne Myths
Many teenage clients believe that acne is caused by poor hygiene. However, acne is not caused by dirt; in fact, scrubbing the skin too vigorously or cleansing with harsh soaps or chemicals irritates the skin and can make acne worse. Teenagers should gently cleanse blemish-prone skin two times a day.
They may also believe that their acne is caused by candy, pizza, and French fries. There are studies that show that high carbohydrates, sugar-laden foods, and a diet high in iodides can make acne worse; these types of food, however, do not cause acne.
There is another popular belief among teenage clients that acne products need to sting to work. They should be aware that any product that burns or stings the skin causes irritation and may lead to unnecessary inflammation, which is a key contributor to any acne lesion. The goal of the product should be to calm inflammation in blemish-prone skin.
Skin care professionals may also come across teenage clients that believe that makeup makes acne worse. The simple truth is that it depends on the makeup. It is important to allow the skin to breathe to kill P.acnes bacteria. Consider printing a list of non-comediogenic ingredients for teenage clients to take shopping when they are looking for makeup.
Another common myth with these clients is that acneic skin does not need a moisturizer. With acneic skin, however, the goal is to balance hydration levels within the skin to stop the overproduction of sebum. When hydration levels balance, the skin will stop producing so much oil. The best results are seen when the moisturizer is formulated with keratolytic, anti-inflammatory, and antibacterial ingredients.
With teenage clients, compliance is the key to gaining the upper hand on acne. Teenagers should continue scheduled treatments with their skin care professional and stick to their daily homecare regimen. Thirty to 40 percent of skin care improvements occur due to professional treatments, the other 60 to 70 percent depends on the teenager. Professionals should have a good relationship established with a dermatologist for those teenagers that may need medical intervention.
Tips for controlling and improving acne include practicing healthy hygiene habits; keeping the hands clean and away from the face; a sufficient amount of sleep; blue LED lights to kill bacteria and red LED lights to calm inflammation; and the use of topicals with salicylic acid, BPOs, and sulfur.
Other tips include washing pillowcases and sheets regularly to kill bacteria; cleaning makeup brushes on a regular basis; taking probiotics during antibiotic use for a healthy intestinal balance; controlling stress; eating a low glycemic diet; talking to the doctor about birth control that balances hormone levels; optimizing vitamin D levels for a healthy immune system that fights infection; and getting professional exfoliation on a monthly basis.
Tea tree oil attacks bacteria and limits oil production and jojoba, hemp, borage, primrose, and chia oils have anti-inflammatory effects. Teenage clients should be patient as it may take four to eight weeks to see results. If they do not see improvement after eight weeks, they should see a dermatologist.
 Medical Procedures for Treating Acne Scars
Medical Procedures for Treating Acne Scars
Some medical procedures for treating acne scars might include soft tissue fillers to even out the skin tone for ice pick scarring, although results are temporary; light therapy, lasers, IPL, and radio frequency, heat the dermis and stimulate the wound healing process without injuring the epidermis; medium depth chemical peels which reach the papillary dermis. Minimize and improve the appearance of scars; punch incision is a minor procedure, the physician cuts out the actual scar and either stitches it shut or closes it with a skin graph; laser resurfacing, lasers can penetrate deep into the dermis to correct textural scarring; extractions on white heads and blackheads only, teenagers should always leave extractions to the professionals to prevent scarring; dermabrasion, normally reserved for severe scarring, sands through the epidermis to blend scarring with the surrounding skin; and steroid injections for nodules and cysts can be performed by a medical professional to immediately flatten the lesion.
Do not allow acne to define teenage clients. Instead, arm them with the products, treatments, knowledge, and tools to take on acne and win.
References
1. Ritvo, E., Del Rosso, J.Q., Stillman, M.A., et al. (2011). Psychosocial judgements and perceptions of adolescents with acne vulgaris: A blinded, controlled comparison of adult and peer evaluations. BioPsychoSocial Med, 5, 1–14.
2. Kam, K. (n.d.). Medications That Can Cause Acne.
3. Richter, R. Stanford Medicine. (n.d.). Go to bed.
4. Sleep for Science. (n.d.).
5. Add-Hair. (n.d.). DHT Blockers.
 Brenda Linday is a licensed aesthetician, licensed aesthetic instructor, and certified aesthetic consultant with over 12 years of experience in the medical aesthetic industry. She offers consulting services to medical and aesthetic companies desiring to build strong sales and education teams. She also develops educational and engagement-marketing content for employees, contractors, practitioners, and industry distributors around the world. Linday's passion is to share her wealth of knowledge with other like-minded professionals who believe that education is key to building lasting relationships with clients, making each clinician more successful by increasing client satisfaction.
Brenda Linday is a licensed aesthetician, licensed aesthetic instructor, and certified aesthetic consultant with over 12 years of experience in the medical aesthetic industry. She offers consulting services to medical and aesthetic companies desiring to build strong sales and education teams. She also develops educational and engagement-marketing content for employees, contractors, practitioners, and industry distributors around the world. Linday's passion is to share her wealth of knowledge with other like-minded professionals who believe that education is key to building lasting relationships with clients, making each clinician more successful by increasing client satisfaction.
Want to read more?
Subscribe to one of our monthly plans to continue reading this article.