
Nutritional and dermatological research has demonstrated that specific and key nutrients are required to ensure the physiological functioning and overall health of the skin. This factor is well recognized by nutritional professionals, along with the premise that simply consuming a balanced diet may not always ensure optimum nutritional status with anticipated benefits or results. Within the realm of nutritional information, there remains one focal determinant of nutrition that is constant no matter the opinion, philosophy, or mindset.

With regard to factors involving nutritional status and the skin, there are a myriad of nutritional philosophies, trend protocols, and self-designed hypotheses from philosophical perspectives – all of which are intended to create healthy, beautiful skin. However, there are important realities of great significance, including bio-individuality and biochemistry. Two subjects may be the same age with general good health and a diet that consists of “eating well.” One subject, however, may have poor nutritional status due to genetic constitution and, as a result, certain nutritional recommendations without clinical assessment may possibly prove ineffective or even detrimental. One of the most important aspects of functional nutrition is the vast amount of information laboratory essays provide in identifying nutrient deficiencies and developing dietary programs based on bio-individuality.
It is important to understand the physiological functioning of the skin as the focal point of assessment and treatment. The state of a client’s skin is influenced by health, nutrient imbalances, deficiencies, medications, stress, and the environment. To provide results-oriented treatment and anticipate the same in completion, it is advisable to adopt a more scientific posture and approach in evaluating the functioning of their skin. The factors that are significant in skin assessment are the constitution of the skin, not simply just the skin type.
Consider that most clients have several co-existing skin conditions and that chronological age does not necessarily indicate the health status of the skin. “Skin aging consists of two didactically independent, clinically and biologically, distinct processes. The first is intrinsic skin aging, which represents chronological aging and affects skin in the same pattern it affects all internal organs. The second is extrinsic skin aging, which we view as aged skin and is the result of external factors and environmental influence, mainly chronic sun exposure and ultraviolet (UV) irradiation but also smoking, pollution, sleep deprivation and poor nutrition.”1
PROTEIN FACTORS
Protein remains a core component in skin health and represents the primary constituent in building cells. The protein people consume as food is broken down by the digestive system, converting food into amino acids to enter the bloodstream. Each cell in the body collects critical amino acids and then utilizes the required protein for bodily functions, including building structure, organs, tissues, and skin.
All metabolic processes are dependent on activity from various proteins. Proteins fuel enzymes that assist in generating power for the body and rely on metabolic sequencing. Metabolic sequencing in cellular chemistry requires that cells possess an active, yet specific, enzyme to be in correct positioning in order to coordinate sequencing of metabolic reactions from nutrients.
There are more than 50 amino acids supplied by proteins and typically 100 to 10,000 amino acids are linked together as chains to form structural units and fibrous proteins: skin, tendons, bone, and muscle.
One-third of the protein content in the body is made up of collagen, which is the major fibrous protein found in the extracellular matrix and connective tissue. Collagen is formed by the triple helix of amino acids – glycine, proline, and hydroxyproline – and, along with keratin and elastin, give the skin its strength. Amino acids are essential for both dermal and epidermal structures and produce the extracellular proteins and enzymes needed for the synthesis of the epidermal barrier. By age 50, many women may lose up to half of the collagen from their skin, which may be compounded to a larger extent by not consuming enough protein for an extended period of time. Protein deficiency can also lead to muscle wasting, poor wound healing, frequent infections, swelling under the eyes and ankles, hair breakage, and hair loss. The quality of protein is extremely important, as well as the frequency of consumption; many sports nutritionists endorse the intake of protein every three hours as it is vitally important to protein muscle synthesis.
VITAMIN C
Vitamin C is a normal skin constituent that is found in high levels of the dermis and the epidermis, however, the content is generally higher in the epidermis. Specific transport proteins for ascorbic acid are found on cells in all layers of the skin and keratinocytes, which have high potential for transport, possibly to compensate for limited vascularization of the epidermis.3
Vitamin C is a critical co-factor for lysyl oxidase and prolyl hydroxylase, which are required to stabilize the triple helical structure of collagen and its crosslink formation.

Ultraviolet light decreases the vitamin C content of the skin, which is influenced by intensity and duration of exposure. The antioxidant activity of vitamin C helps to protect the skin from ultraviolet damage resulting from free radicals, potentially reduce ultraviolet-related DNA damage and lipid peroxidation, limit the release of pro-inflammatory cytokines, and protect against cell apoptosis.3
Nutritional intake of vitamin C is imperative since vitamin C is not naturally synthesized by the human body. Some nutrient-dense sources of vitamin C include citrus fruits, strawberries, kiwi, blackcurrant, rose hip, guava, broccoli, kale, brussel sprouts, peppers, and parsley.

VITAMIN A
Dietary vitamin A is presented in two forms: active vitamin A and beta carotene. Vitamin A is derived from animal foods, called retinol, and can be used directly by the body.

Beta carotene metabolism takes place in a number of organs, including the skin.6 With dietary supplementation, beta carotene can be further enhanced in the skin and the bioavailability of provitamin A and retinol can be increased by essential fatty acid status. Dietary sources of vitamin A include: apricot, beef, butter, broccoli, chicken, carrot, cheddar cheese, cod liver oil, eggs, fish liver, kale, milk, mangos, spinach, pork, peas, pumpkin, sweet potato, and turkey.
Vitamin A is essential for supporting immune function and eye health, aids in fighting inflammation and cellular damage, and even assist in the suppression of cancer.7
In the skin, retinol is converted to retinaldehyde and then to retinoic acid. Retinoic acid modulates gene expressions and influences cellular processes in both the dermis and the epidermis. Vitamin A influences epidermal differentiation, modulating growth factors, inhibiting sebaceous gland activity, and suppressing androgen formation.5 Cutaneous effects of vitamin A deficiency affects epithelial tissue, increases keratinization, and facilitates delayed wound healing.
Vitamin A has documented photoprotective properties – cutaneous absorption of vitamin A via retinyl esters concentrated in the epidermis will absorb ultraviolet radiation at 325 nanometers. Thymine dimer formation is a primary marker of DNA damage and represents a risk for the potential development of skin cancer as a result of UVB-induced erythema. Topical retinyl palmitate has been shown to inhibit thymine dimer formation through compounded doses acting as a filter against ultraviolet radiation.8 Retinyl palmitate will increase collagen and enhance DNA, skin thickness, and elasticity.
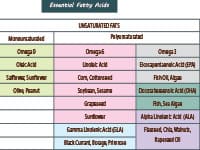
ESSENTIAL FATTY ACIDS AND LIPIDS
The epidermis is organizational and divided into specific cell types and lipid composition. As cellular differentiation occurs – keratinocytes are metabolically active due to essential fatty acids and epidermal phospholipids. Lamellar bodies (differentiating keratinocytes) deliver essential lipids to the stratum corneum. The stratum corneum is encased in a protein and lipid matrix, a juncture that is essential to the barrier function of the skin.
Cutaneous aspects and functions of essential fatty acids play a major role in skin functioning and health: intercellular cohesion, superficial lipid film, cell membrane fluidity, and precursors for eicosanoid anti-inflammatory mediators.17
Lipids are synthesized from amino acids, carbohydrates, and phospholipids and include saturated fatty acids, monosaturated fatty acids, cholesterol, and ceramides, which can be modified and synthesized by the skin. Essential fatty acids are functional components with regard to both the dermis and epidermis, are a form of polyunsaturated fats that cannot be synthesized by the human body, and must be obtained from various and specific foods. An essential fatty acid deficiency can produce severe cutaneous abnormalities by affecting both function and appearance, including hyperproliferation of the epidermis, transepidermal water loss, and dermatitis. Transepidermal water loss is directly related to structural cell lipids and essential fatty acids – biochemical evidence of essential fatty acid deficiency can be determined from just a few days to weeks. Symptoms include: dryness, scaling, flaking, itching, increased sensitivity, keratosis pilaris, and potential rashes.
WATER AND HYDRATION
Water is the most essential nutrient – cells consists of approximately 55 to 78 percent water, depending on the person’s age, body size, and gender; the skin contains about 70 percent water. Cellular hydration and a healthy framework of the epidermis is dependent on water intake. Lack of sufficient water in the tissues will impede transfer of fluids and affect the elimination system, including the skin. When cellular dehydration occurs, it triggers a catabolic state where water leaves the cells in order to maintain blood volume and pressure.
This reaction can result in accelerated aging, DNA damage, muscle damage, and susceptibility to free radical damage.
Imbalances related to cellular dehydration include headaches, joint and muscle pain, dry skin, eczema, psoriasis, dry eyes, constipation, food sensitivities, mood swings, poor energy and sleep, sugar cravings, fluid retention, weight issues, and abnormal blood pressure.9 When cellular hydration is restored, cells expand and healing mechanisms are enhanced; reduction of cellular acidity creates a more alkaline state, increase in fat burning, and DNA repair.10
MICROBIOME
In more recent years, the topic of prebiotics, probiotics, and the microbiome have become of heightened interest to skin care professionals.

The gut-skin connection has become a major consideration when evaluating potential origins for multiple skin conditions. The gut flora (or microbiota) is a general community and ecosystem where approximately 300 to 500 species of bacteria reside and communicate within the gastrointestinal track and the immune system.11 In any given portion of the gut, the composition and balance of the flora may interact with the mucosal surface of the organs, various bacteria, and the immune system – which may be instigated in compromised situations – such as gastrointestinal, digestive, and stomach disorders, depending on health status and dietary changes.
Prebiotics
Prebiotics are foods that contain non-digestible fibers and encourage the growth of beneficial microorganisms in the microbiota. These foods help to naturally boost the immune system and improve metabolic health by passing through the upper portion of the digestive tract and colonizing good bacteria to act as a substrate for the large bowel. Natural prebiotics include chicory root, dandelion greens, Jerusalem artichoke, garlic, onions, leeks, asparagus, bananas, barley, oats, apples, cocoa, burdock root, flaxseeds, wheat bran, and seaweed.
Probiotics
Probiotics are live bacteria that naturally occur in certain foods, such as sauerkraut, fermented vegetables, and yogurt. They are also beneficial organisms found in the gastrointestinal tract and work to promote health at the cellular level, aid in regulating immune responses, and promote function of the intestinal inner lining. The word probiotic means “promoting life.” They are cultured in countless food sources and supplements. Pharmabiotics use probiotics as natural pharmaceutical agents in the treatment and prevention of disease.15
Probiotics are an important nutritive substance that are staples in wellness, health, and nutrition programs throughout the world. The 
With regard to the skin, there has been an increase in the amount of research outlining the connection to the microflora of the skin and the gastrointestinal tract. Leaky gut syndrome, SIBO, and general digestive disorders have been connected to eczema, psoriasis, acne, dermatitis, rosacea, and even hives. Furthermore, skin infections and faulty microbial defense systems may lead to pathogenic and secondary infections.
According to Dr. Ralph Kellman of the Center for Functional and Integrative Medicine, the skin microbiome confers immunity by starving out invaders for competition for nutrients; blanketing the skin’s surface by crowding out pathogens; altering and educating immune cells; influencing the development of T cells and antigen-presenting cells; secreting antimicrobial substances that fight and destroy invaders; and changing the local environment, concluding in a protective effect.12
Consider the microflora of the skin as a main chemical and antimicrobial defense system. Impaired immunity can affect and disrupt the integrity of the epidermis and barrier function. Many forms of stress disrupts the ability of the protective mechanism of the stratum corneum and triggers adaptive response of the hypothalamic-pituitary-adrenal axis to release hormones and pro-inflammatory ytokines.14
skin’s capacity to resist infection, not necessarily the inherent properties of the microbe itself.13 The physical barrier defense of the skin will activate via a hostile surface pH and conditions conducive to inflammation and infection.
The importance of key nutrients, supportive catalysts, and essential components serve that as support mechanisms to help maintain healthy skin cannot be underestimated. The individual benefits of these nutrients is indeed established, however, it is the total sum and the interrelationships of these components that are beneficial to overall skin homeostasis.
References
1. Schagen, S. K., Zampeli, V. A., Makrantonaki, E., Zouboulis, C. C. (2012, April 3) Discovering the link between nutrition and skin aging. Dermato-Endocrinology, 298–307.
2. Michels, A. J. (2011, September). Vitamin C and skin health. Linus Pauling Institute. Oregon University.
3. Pumori, S.T. Vitamin C in dermatology. (2013, April) Indian Dermatol Online Journal, 143–146.
4. Chen, M. C., Hsu, S. L., Lin, H., & Yang, T. Y. (2014, April 22). Retinoic acid and cancer treatment. PubMed. NCBI.
5. Shils, M. E., & Shike, M. (2006). Modern nutrition in health and disease. Google Books.
6. Antille, C., Tran, C., Sorg, O., Carraux, P., Didierjean, L., & Saurat, J. (2003). Vitamin A exerts a photoprotective action in skin by absorbing ultraviolet B radiation. Journal of Investigative Dermatology, 121(5), 1163-1167.
7. Zoovetvaru. (n.d.). Fatty acids in dermatology.
8. Wellbeing with Nutrition. (2013, December 23). Cellular dehydration: Causes and effects.
9. Lavina, A. (2016). The importance of cellular hydration and nutrition. QBuzz.
10. Quigley E. (2013, September) Gut bacteria in health and disease. Gastroenterol Hepatol, 560–569.
11. Killian, J. (2012, April). The overlooked role of probiotics in human health. Life Extension, 1.
12. California Dairy Research Foundation. (n.d.). Probiotics basics.
13. Kellman, R. (n.d.). Skin microbiome. The unseen warrior. Prebiotics for Skin Care. Kellman Center, 1.
14. Slominski A. (2007) A nervous breakdown in the skin: stress and the epidermal barrier. J Clin Invest, 117:3166–9.
15. Cogen A. L., Nizet V. & Gallo R. L. (2008) Skin microbiota: a source of disease or defence? Br. J. Dermatol. 158, 442–455.
16. Draelos ZD. (2010) Nutrition and enhancing youthful-appearing skin. Clin Dermatol. 28:400–8.


























0 Comments