Inflammation:
(L. inflammare, from flamma, flame) The complicated physiological process in mobilization of body defenses against foreign substances and infection agents, and repair damage from such agents.
Inflammatory Response:
A complex series of interactions between fragments of damaged cells, surrounding tissues, circulating blood cells and specific antibodies; typical of infection.
The Immune Response – Inflammation
The signs of inflammation are redness, swelling, heat and pain with an inability for normal cells to function correctly. Inflammation occurs only in vascular tissues.3 The purpose of the inflammatory response is to mobilize the body's defenses against infection.4 The biological signs of inflammation are due to a deluge of plasma from blood vessels into affected tissue, along with the passage of leukocytes (white blood cells) into the site of injury.5 There is an increased of vascular permeability that allows for immune cells to enter through the walls of blood vessels to the damaged area. A cascade of responses and activation of blood plasma enzymatic systems fight off the infection.6 Wound healing response is determined through the degree of damage and/or infection. The presence of numerous mediators such as fibroblasts, macrophages, mast cells, monocytes, lymphocytes and others stimulate systemic response to the inflammatory process that can include fever and even lower blood pressure or in severe allergy reactions, anaphylaxis shock. Additionally, cytokines also influence the inflammatory response.
The body is genetically programmed to take care of itself. Its millions of cells communicate with one another through cell receptors and know when to rebuild tissue and when to perform apoptosis (cell death) and remove the debris. It is a remarkable process that is scarcely understood 100 percent by even the greatest of scientists. The body has a vast defense system that can hinder interlopers (bacteria, viruses) from causing irreversible harm that could lead to death of the organism. Torn and hurt tissue immediately recruits an army of workers that go to the sight of injury to help repair, rebuild and take away the debris. Cell supervisors manage these processes and send signals to stop the repair process upon job completion.
At every microsecond the body readjusts itself to compromise for both internal and environmental influences. Our innate immune system is what keeps us alive through its thousands of genetically directed programs that communicate with one another producing signals throughout the trillions of cells that all miraculously know on a healthy day and what to do in the event of invasion, injury or chronic disease. The immune system knows what is foreign and what is friendly.7 It requires balance and T-1 helper cells and T-2 cells help regulate the body's response to bacteria, and viruses (antigens) that have foreign proteins or polysaccharides on their outer surface.8 The T-1 cells (derived in the thymus) stimulate white blood cells to attack viruses and cancer cells. The T-2 cells use antibodies to destroy bacteria. The immune system has the ability to build specific proteins called antibodies (B-cells propagate antibodies) that can fight these antigens in the event of reoccurrence.9
The body has three innate levels of powerful defense groups antioxidants, DNA repair and Cell death.10
Cytokines and the Immune Response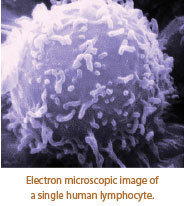
Cytokines (or lymphokines) are a special family of molecules that are primarily secreted from immune cells called leukocytes.11 The action of the cytokines is required on a daily basis. Cytokine activity occurs in steps and thus it interacts with a cell receptor and activates or stimulates the receptor to produce an end result.12 Cytokines orchestrate, coordinate and support the body's ability to fight off pathogens, repair damage, and restore and maintain cellular health.13 They also make up groups of compounds called interleukins. Many cytokines are called "growth factors" and are chemicals that stimulate cells to divide and grow.14 Cytokines can elicit their effects at the site of injury or even systemically. They can both give positive and negative effects. When a cell is damaged or infected with microbes cytokines release chemokines that summon an influx of white blood cells. Other cytokines can encourage injured cells to emit toxic, microbicidal chemicals and enzymes to ingest both the microbes and injured tissue.15 They can also create an inflammatory response, especially when there are major assaults on cells and systems as in the case of disease, sunburn, and glycation (a pathological process in the body that causes inflammation showing up as deep wrinkles and poor skin quality16). Cytokines can be involved in very acute inflammation and can trigger fever through enhancing prostaglandin E2. This also elicits histamine from mast cells causing vasodilation and more inflammation.
Cytokines - Autoimmune Diseases and Aging
The body will do its best to compensate during times of stress since it was designed to do this under numerous circumstances. However, chronic disease is another story that can sometimes overtake this normal process. There are over 100 autoimmune disorders: i.e., Lupus, Addison's Disease, Asthma, Atopic Dermatitis, Diabetes types 1 and 2; Fibromyalgia, Grave's Disease, et cetera.17 While cytokines are part of the normal immune response, there are theories that overproduction of these cytokine molecules leads to an invasion and inflammation of a body organ or system. When things get out of control, a ground swell of inflammation occurs that does not turn off. Inflammation becomes chronic. For example, in the life of a diabetic the inflammation process continues day after day eventually leading to a cascade of events that impair quality of life. Furthermore, rheumatoid arthritis cascades into crippling, debilitating joints and diminishing of quality of life as the patient tends with the disease. Additionally, over production of cytokines has been targeted as a contributing factor for mood disorders such as depression, anxiety, or anorexia.18
Aging
Aging is considered a cellular response to oxidative stress that alters cell-signaling pathways including the chondrocytes (Greek chondros = cartilage + kytos = cell) that can disrupt the response to growth factors.19 Research shows that excessive oxidative stress alters energy production leading to premature cell death in osteoarthritic cartilage resulting in osteoarthritis.20 Additionally, aging correlates with reduction in regulatory-type cytokines and T cells found in the gut mucosa.21 Cell mitochondria are also greatly affected.
The Mitochondria
The mitochondria are the main energy source in the cell responsible for cell respiration. Due to their high activity in producing energy, they also become an essential source of reactive oxygen species (ROS).22 Mutations occur more frequently in mitochondria DNA due to its limited repair system. There are more than 20 known diseases associated with abnormal DNA including diabetes, Alzheimer, Parkinson, heart and muscle disease.23 Excessive amount of oxidative stress (free radicals) is caused by influences such as lifestyle including pollution, smoking, excessive UV exposure, stress, sleep deprivation, poor food choices (especially sugars and refined foods), and obesity. You can easily assume that oxidative stress and mitochondria damage is the true reason behind wrinkled and poor quality skin.
Tissue Response to Wound Healing
Let us summarize the steps of the wound healing process:
Coagulation and Inflammatory Phase (1 to 3 Days)24:
In the event of an open injury (cut, abrasion, laceration) the immune response goes through numerous phases to close up the opening to prevent invasion of bacteria and then continues to remodel the skin. The "inflammation" seen during this process is a result of what is called "first responders"25 that seal off the area forming a clot. The redness and swelling is a result of this process since white blood cells (neutrophils and lymphocytes) flood the area in order to catch bacteria. The area is "cleaned" with the macrophages engulfing the damaged tissue and debris removing it away from the area. This process is known as phagocytosis.
Proliferative Phase (3 to 5 Days):
The first responders recruit the repair cells – fibroblasts and endothelial and epithelial cells. New blood vessels are formed (angiogenesis) to replace the damaged ones and to act as a transport for building materials and removal of waste from building new tissue. Initially there is an over abundance of blood vessels to cope with the increased oxygen demands of the repair process. Eventually they are destroyed once they are not required. A wound must be hastily closed so new collagen type III is produced to form granulation tissue.26
Fibroblastic Phase (5 to 20 Days):
The inflammatory phase reduces as the wounding process is altered for new tissue formation. With the help of growth factors, the wound enters into the fibroplastic phase to produce new tissue at the wound site. A glycoprotein called fibronectin binds to the wound matrix to act as a conduit for the fibrolast cells to fill the space.27
Maturative and Remodeling Phase (28 Days to 2 years):
Collagen protein makes up the extracellular matrix and including about 50 percent of the scar tissue. In the early stages of wound healing, collagen is quickly laid down in a less organized manner. Over time, cross links of peptide chains are developed during this final stage of remodeling whereby collagenase (enzyme) breaks down inappropriately oriented collagen molecules. A less traumatized collagen is the result providing strength and smoother texture.28
Supporting Healthy Skin – the Role of the Aesthetician
Throughout our daily aesthetic practice, we utilize numerous treatment modalities to render correction to various skin conditions. They include acne, pigmentation, excess (or lack of) lipid secretions, vascular (rosacea, telangiectasia), imbalances caused by an impaired acid mantle, oxidative stress (free radicals), lack of free water, and glycation (severe damage to underlying dermal structures - rete pegs [connective tissue between the epidermis and dermis], collagen and elastin). All of these conditions create inflammation. At every moment, the skin is constantly adjusting itself in order to adhere to the delicate equilibrium and balance so necessary for optimum function and immune protection. How do we recognize skin that is healthy and free from major challenges?
The Analysis
Appearance is the first sign that provides a quick visual that conveys the health of the skin. One just has to observe the skin of a baby or small child to gain a perspective of beautiful skin. Younger skin can serve as a benchmark for measuring the accumulative effects of what happens to skin that is environmentally exposed and/or neglected. The skin analysis requires you to observe several aspects. A trained eye can quickly assess depth of damage. Is the skin smooth, firm, evenly pigmented, adequately hydrated, and possess an intact skin barrier defense?29 Is the skin resilient, rich in collagen and elastin? Does it have a dense spinosum layer with consistent, strong cell-to-cell (desmosomal) adhesion? Does it have healthy bi-layers that support slow evaporation of the natural moisturizing factor (NMF)?
Keratinocyte cells cross-talk (signal) with one another in order to maintain a strong barrier function.30 They interact with the immune system and send signals to the basal layer and intercellular areas. They support the manufacturing of the lipids found within the bi-layers that act as "waterproofing" and germicidal. Moreover, recent research has uncovered hundreds of tasks that are performed by the keratinocytes that interact with the immune system (Langerhans), the melanocytes, and the numerous enzyme processes that are catalyst for other cell functions. Keratinocyte function cannot be looked upon lightly because they have a huge responsibility in maintaining the integrity and health of
the epidermis.
 Restore and Repair
Restore and Repair
The role of the skin care professional is to support the health of this skin barrier through restoring the first three lines of skin barrier defense – (1) the acid mantle, (2) corneocytes (straum corneum), (3) lipid bilayers.31 Next are the keratinocytes to improve epidermal density and stimulate proper keratinization for a smoother and more compact stratum corneum and also results in a strong barrier function.32 Additionally, melanocytes are targeted to improve a more even skin color. The fibroblasts can gently be stimulated to produce quality collagen, elastin and glyosaminoglycans (GAGs) for a firmer, tighter skin.33
This is accomplished through carefully considered and monitored treatments along with educating the patient/client to provide a logical program to ensure that more damage is not rendered to skin that may be already compromised. It is wiser to restore the skin first prior to moving on to more aggressive treatments. A huge common mistake is that we are too anxious to delve into aggressive treatments without realizing that we must spend the first four to seven weeks of treatment in repairing the acid mantle and supply the skin cells with the essential building blocks they require through oral nutrition and supplements, topical creams, serums and other repair products along with gentle in-clinic treatments.34 While the first impulse is to reach for the peel bottle, microdermabrasion or even a laser, a healthier approach for repair is to clearly understand each skin condition, the health of the client, and to customize a system that restores the skin gradually. The slightest skin treatment can interrupt the thousands of signals and intercommunication occurring within the epidermal components. The more invasive the treatment the more interruption there is within both the epidermis and dermis due to inflammation.
Conclusion
Simply said, inflammation is a process by which the normal cell functioning within the body is interrupted and/or impaired cascading into a mode of response, which means that the immune system will do what is required to fight off any infection or sudden injury to itself. Normal immune response is a natural defense that the body controls itself through its innate genetic programming. This response can be very small, such as when we have a fissure on our fingertips to something very large such as a major injury and disease. Oxidative stress (as mentioned earlier) is a key culprit in accelerating the aging process due to its affect on cells and systems. A greater insight to preventing excessive inflammation in biological aging is the awareness that lifestyle, thoughts, nutrition and daily choices enhance our overall quality of life. It is the difference between why one individual gets sick and why one recovers.
Resources:
1 Pugliese, P. M.D. (2005) Advanced Professional Skin Care –
Medical Edition, p. 421
2 IBID
3 IBID. p. 165
4 IBID, p. 176
5 IBID, p. 165
6 IBID, p. 165
7 IBID, p. 145
8 IBID, p. 146
9 IBID, 146
10 Draelos, Z.MD, Pugliese, P.T., MD (2011) Physiology of the Skin, Third Edition. p. 429-431
11 IBID – See Reference 1 - p. 163
12 IBID p. 162
13 IBID p. 160
14 IBID p. 161
15 IBID p. 160
16 IBID p. 541-542
17 List of Autoimmune Diseases Retrieved from
http://www.squidoo.com/list_of_autoimmune_diseases
18 Anisman, H, Merall, Z. Cytokines, stress and depressive illness: brain-immune interactions. Ann Med. 2003:35 (1):2-11 Retrieved from http://www.ncbi.nlm.nih.gov/pubmed/12693607
19 Loeser, R.F. Aging and osteoarthritis. Curr Opin Rheumatol, 2011 June 30. Retrieved http://www.ncbi.nlm.nih.gov/pubmed/21709557
20 IBID See Reference 17
21 IBID
22 Draelos, Z.MD, Pugliese, P.T., MD (2011) Physiology of the Skin,
Third Edition. p. 424-427
23 IBID p. 431
24 Setterfield, L. M.D. (2011) The Concise Guide Dermal Needling – Medical Edition. Virtual Beauty, New Zealand.
ISBN 978—0-473-17321-0
25 IBID
26 IBID
27 IBID p. 32-33
28 IBID p. 32-33
29 Barrett-Hill, F. (2004) Advanced Professional Skin Care: Understanding Skin
Physiology. Virtual Beauty, New Zealand. ISBN 0-476-00665-1
30 IBID – Setterfield – See 23
31 IBID p. 6-7
32 IBID
33 IBID
34 IBID p. 2-3
 Alexandra J. Zani is an international educator with a background in biology and medical technology. She holds a teaching license for cosmetology/aesthetics, is NCEA nationally certified, and an independent technical and scientific advisor for postgraduate studies in the medical spa industry, including cosmeceutical development. Zani presents education for advanced aesthetic technology including: Microcurrent, LED and laser. She is a specialist in the anti-aging sciences, including the affects of nutrition, lifestyle and the mind/body connection. Presently, Zani facilitates and teaches post-graduate aesthetics education, is a technical writer, and consultant and a founding member of the International Organization of Continuing Education Providers (IOCEP). She is a contributing author for textbooks and industry publications. She is co-author with E.A. Ordonez, M.D. of a newly released book "Eat to be Free." This email address is being protected from spambots. You need JavaScript enabled to view it.
Alexandra J. Zani is an international educator with a background in biology and medical technology. She holds a teaching license for cosmetology/aesthetics, is NCEA nationally certified, and an independent technical and scientific advisor for postgraduate studies in the medical spa industry, including cosmeceutical development. Zani presents education for advanced aesthetic technology including: Microcurrent, LED and laser. She is a specialist in the anti-aging sciences, including the affects of nutrition, lifestyle and the mind/body connection. Presently, Zani facilitates and teaches post-graduate aesthetics education, is a technical writer, and consultant and a founding member of the International Organization of Continuing Education Providers (IOCEP). She is a contributing author for textbooks and industry publications. She is co-author with E.A. Ordonez, M.D. of a newly released book "Eat to be Free." This email address is being protected from spambots. You need JavaScript enabled to view it.
Want to read more?
Subscribe to one of our monthly plans to continue reading this article.