
Having an understanding of how hormones affect the skin can help licensed practitioners assess the causes of some skin conditions and should be included in dialog during the initial consultation. Discussing the effects of hormones during the consultation will help give the client a clearer picture to some causes of their skin concerns.
WHAT ARE HORMONES?
Hormones are chemicals secreted by cells or glands, which act as messengers that are sent out from one part of the body to signal cells in other parts of the body. Hormones control and regulate the body’s internal environment by regulating metabolism, controlling the reproductive cycle, inducing hunger and cravings, stimulating or inhibiting growth, and preparing the body for changes such as puberty, childbirth, or menopause. They are often released directly into the bloodstream, but may also be secreted into ducts.
THE EFFECTS OF INFLAMMATION
Inflammation is a process by which the body’s white blood cells and chemicals protect us from infection such as bacteria and viruses. However, inflammation is also the single greatest precipitator of aging and age-related diseases and does damage by stimulating free radicals, which accelerates aging by attaching to and damaging cells. With acne, the stimulation of the oil glands, brought on by pro-inflammatory responses, can result in clogged pores and an increase in pro-inflammatory fatty acids. Studies have shown that there is a connection between sugar and inflammation in the body.

Other factors to consider are the effects that stress has on hormones. Systemically, stress stimulates hormones which can affect acne breakouts. Elevated hormone levels prior to menstruation, or excessive androgen (male sex hormone) production produced by the adrenal glands, can make acneic conditions worse in both men and women. Women are more affected than men by pro-inflammatory responses related to cortisol and insulin and the effects of androgens in the body. A woman’s androgens are synthesized in the adrenal glands; therefore, they are more susceptible to adrenal hormone stimulation and more prone to inflammatory responses in the body. Hyperandrogenism may be caused by disorders such as polycystic ovarian disease, which can indicate insulin resistance with acne patients.
TREATMENT FOR EXCESSIVE ANDROGEN LEVELS, HORMONAL IMBALANCE
Prescription drugs such as low-dose estrogen birth control pills can help reduce androgens produced by the ovaries, whereas, low-dose corticosteroids can be used to suppress androgen produced by the adrenal glands. Anti-androgen drugs can be used to reduce excessive oil and sebum production, but do have associated side effects. Vitamins such as B6 help maintain blood glucose levels within a normal range and may help reduce inflammation in the body. A vitamin such as B5 reduces inflammation and stress responses and also balances hormones needed for proper function of the adrenal glands.

Acne
As the body begins to develop and goes through puberty, conditions such as acne begin to surface. Hormone levels directly affect the rate at which sebocyte enzymes synthesize lipids. As sebocytes differentiate and mature, they accumulate, increasing the amounts of lipids. With time, mature sebocytes migrate toward the central excretory duct of the sebaceous gland and eventually break apart, releasing their lipidic contents. These lipids and disintegrated sebocytes are then released through the excretory duct onto the skin. The activity and size of the sebaceous glands can vary according to circulating hormone levels and age. With acne, the effects of stress and inflammatory responses should be considered.
Aging
With age, the body produces lower levels of hormones and hormones lose their ability to communicate messages. This miscommunication, also known as hormone miscommunication, can cause an imbalance in the endocrine system, accelerating the aging process. Hormone miscommunication can occur when the body is under constant physical and emotional stress.
The results of hormone miscommunication are:
- Excess Blood Glucose – destroys collagen
- Excessive Free Radicals – oxidative damage to cells
- Increase in Insulin Resistance – body cannot recognize insulin
- Increased Cortisol Levels – stress hormone which causes increase in blood sugar
- Immune Function and Longevity
With age, there is a deterioration of immune response in the body. Among others, this deterioration is a result of continuous exposure to viruses, bacteria, pollution, and food. In middle age, this exposure is accelerated by increased levels of hormones such as cortisol and decreased levels of DHEA. A decrease in immune responsiveness is also linked to an overproduction of inflammatory cytokines, which makes inflammation the largest contributor to aging and disease. This is why an anti-inflammatory diet should be considered.
Anti-inflammatory Diet: Essential to Health
An anti-inflammatory diet will help prevent and reverse oxidative damage caused by free radicals on a cellular level and is essential to aging and total body health. Studies have shown that anti-inflammatory foods and antioxidants are key to preventing intrinsic aging and disease.

Research has suggested that estrogen deficiencies following menopause may contribute to aging in skin. Although the exact mechanisms are not known, the reduction in estrogen is believed to increase skin thickness, dryness, and loss of elasticity.
Estrogen receptors have been detected in the skin, which makes topical estrogens effective in treating aging skin. Topical estrogens have been shown to have antioxidant properties and have anti-aging benefits. Phytoestrogens, found in plants, have shown to mimic estrogen and have antioxidant affects.

Keratosis pilaris, an excessive buildup of keratin within the hair follicle, is a genetic skin disorder. Keratosis pilaris is a benign condition that appears like tiny tan, red, or white bumps that occur on the upper arms, legs, buttocks, or cheeks and is often associated with other dry skin conditions such as eczema and ichthyosis. Keratosis pilaris affects adolescents during puberty, but can also occur in adults. Keratosis pilaris affects nearly 50 to 80 percent of all adolescents and approximately 40 percent of adults and is believed to be linked to hormonal fluctuations, as well as imbalances. Keratosis pilaris may occur when there is an excess of estrogen in ratio to progesterone, if ovulation does not take place, or if there is insufficient progesterone due to a defective luteal phase. Keratosis pilaris is commonly found during hormone fluctuations that occur during pregnancy or menopause, as well as with hormone replacement therapy.
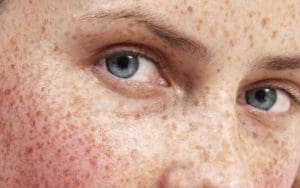
Post-Inflammatory Hyperpigmentation
The process of inflammation is a contributing factor to post-inflammatory hyperpigmentation. When treating inflamed acne or dark skin phototypes, reducing inflammation and inflammatory responses of white blood cells should be considered in order to reduce risk factors to post-inflammatory hyperpigmentation. Women are most affected by pro-inflammatory responses and the effects of androgens in the body and are more susceptible to adrenal hormone stimulation. The effects of androgens in the body should be considered as a risk factor to post-inflammatory hyperpigmentation.

Melasma, also known as chloasma, is a tan or dark facial skin discoloration. It is one of the most challenging skin conditions to treat and can reappear. Melasma appears as dark irregular patches which are commonly found on the upper cheek, nose, lips, upper lip, and forearm. These patches usually develop gradually over time and do not cause concern for any other symptoms beyond cosmetic discoloration. With melasma, there are numerous factors to consider, as well as underlying conditions that trigger hormonal responses.
Melasma and Ethnicity
Melasma is most prevalent in men and women of darker skin colors, or those of Fitzpatrick skin phototypes III to VI. With melasma, ethnicity should also be considered. The occurrence of melasma is commonly found with people of Native American, German, Russian, or Jewish decent. When treating melasma, both skin color and genetic predisposition should be considered. With lighter skin types, predisposed factors such as ethnicity should be an important consideration as well, which can contribute to an increase of melanocyte activity and melasma. With an increase of melanocyte activity, individuals with darker skin types such as African, Hispanic, Indian, Middle Eastern, Mediterranean and Asian are at a greater risk to melasma and hyperpigmented disorders. Individuals who are most susceptible to melasma are women who have a light brown skin type and have had been exposed to intense sun.
Hormones, Medications and Melasma
Melasma is a condition that is commonly found in pregnant women, women taking oral contraceptives, or women on hormone replacement therapy (HRT). In pregnant women, melasma tends to fade post-partum, but can return with subsequent pregnancies. The discoloration will usually disappear over a period of several months after giving birth. On the other hand, melasma caused by oral contraceptive use typically does not fade after discontinuing use of the drug.

There are certain medical conditions that can bring the onset of melasma and can increase in patients with thyroid disease. With endocrine disorders such as Addison’s disease, a minor injury can stimulate the onset of melasma.
Melanocyte Stimulating Hormone and Stress
It is thought that the overproduction of the melanocyte stimulating hormone (MSH), brought on by stress, can cause outbreaks of melasma. Other rare causes of melasma include allergic reaction to medications and cosmetics. Predisposed factors such as ethnicity should be considered with medications and cosmetics, as well as stress levels which can cause an imbalance in the endocrine system.
Inflammatory Responses Stimulates Melanocyte Activating Hormones
Hormone-like substances commonly called inflammatory mediators activate a wide variety of responses in the skin, including an increased release of histamine and activation of melanocytes. During an inflammatory response or ultraviolet (UV) exposure, the skin may produce as many as eight to 10 different types of melanocyte activating hormones, which bind to specific receptors on the surface of melanocytes, triggering the activation of the cell from its resting state to a melanin-producing, active state.
The Effects of Ultraviolet Radiation: Exasperating Melasma
Ultraviolet radiation contributes to the development and the exasperation of melasma. Ultraviolet radiation can cause both an increase in melanin production and transfer, as well as an increase in the number of melanocytes. Individuals with lighter skin types (Fitzpatrick Phototype I to II) and living in an area of high sun exposure are at a high risk of developing melasma, as well as predisposed ethnicities. Years of ultraviolet exposure induces a constant production of inflammatory hormones, ultimately resulting in a permanent activation
of melanocytes.

When treating skin conditions and disorders, the initial consultation, as well as follow-up visits, should include a thorough health history. Predisposed factors such as Fitzpatrick skin phototype and ethnicity should be addressed, as well as considerations such as hormones, lifestyle, diet, and sun exposure. With a thorough understanding of the causes and contributing factors of skin diseases, the licensed practitioner will be able to provide an individual treatment protocol for optimal clinical outcomes.
References
1 Balta I, Ekiz O, Ozuguz P, Sen BB, Balta S, Cakar M, Demirkol S. Nutritional Anemia in Reproductive Age Women with Postadolescent Acne. Cutan Ocul Toxicol. 2013 Sep;32(3):200-3. doi: 10.3109/15569527.2012.751393. Epub 2013 Jan 25. PMID: 23351097 [PubMed – in process]
2 Beylot C. Skin Aging: Clinicopathological Features and Mechanisms. Ann Dermatol Venereol. 2008 Feb;135 Suppl 3:S157-61. doi: 10.1016/S0151-9638(08)70072-3. Review. French. PMID: 18342119 [PubMed – indexed for MEDLINE]
3 Chen W, Obermayer-Pietsch B, Hong JB, Melnik BC, Yamasaki O, Dessinioti C, Ju Q, Liakou AI, Al-Khuzaei Katsambas A, Ring J, Zouboulis CC. Acne-Associated Syndromes: Models for Better Understanding of Acne Pathogenesis. J Eur Acad Dermatol Venereol. 2011 Jun;25(6):637-46. doi: 10.1111/j.1468- 3083.2010.03937.x. Epub 2010.Dec 29. Review. PMID: 21198949 [PubMed – indexed for MEDLINE]
4 Chuan SS, Chang RJ. Polycystic Ovary Syndrome and Acne. Skin Therapy Lett. 2010 Nov-Dec;15(10):1-4. PMID: 21076799 [PubMed – indexed for MEDLINE]
5 Clerkin EP, Sayegh S. Melanosis as the Initial Symptom of Addison’s Disease: A Case Report.
6 Lahey Clin Found Bull. 1967;16(1):173-6. No abstract available. PMID: 6044526 [PubMed – indexed for MEDLINE]
7 Da Cunha MG, Fonseca FL, Machado CD. Androgenic Hormone Profile of Adult Women with Acne. Dermatology.2013;226(2):167-71. doi: 10.1159/000347196. Epub 2013 May 16. PMID: 23689531 [PubMed – in process]
8 Fuller, Bryan B. Ph.D., Scientific Advisor Nu Skin. Causes of Human Skin Hyperpigmentation.
9 Kamangar F, Shinkai K. Acne in the Adult Female Patient: A Practical Approach. Int J Dermatol. 2012. Oct;51(10):1162-7 4. doi:10.1111/j.1365-4632.2012.05519.x. Review. PMID: 22994662 [PubMed – indexed for MEDLINE]
10 Kim NH, Cheong KA, Lee TR, Lee AY. PDZK1 Upregulation in Estrogen-Related Hyperpigmentation in Melasma. J Invest. Dermatol. 2012 Nov;132(11):2622-31. doi: 10.1038/jid.2012.175. Epub 2012 Jun 14. PMID: 22696060 [PubMed – indexed for MEDLINE]
11 Marciniak A, Nawrocka-Rutkowska J, Wiśniewska B, Brodowska A, Starczewski A. Chronic Inflammation and
Metabolic Syndrome in Comparison with other Signs Belonging to the Image of Polycystic Ovary Syndrome. Pol Merkur, Lekarski. 2013 Apr;34(202):228-31. Review. Polish. PMID: 23745331 [PubMed – indexed for MEDLINE]
12 Park JY, Kim YC, Lee ES, Park KC, Kang HY. Acquired Bilateral Melanosis of the Neck in Perimenopausal Women. Br J.Dermatol. 2012 Mar;166(3):662-5. doi: 10.1111/j.1365-2133.2011.10735.x.PMID:22091619 [PubMed – indexed for MEDLINE]
13 Passeron T. Melasma Pathogenesis and Influencing Factors – An Overview of the Latest Research. J Eur Acad Dermatol,Venereol. 2013 Jan;27 Suppl 1:5-6. doi: 10.1111/jdv.12049. Review. PMID: 23205539 [PubMed – indexed for MEDLINE]
14 Sarvjot V, Sharma S, Mishra S, Singh A. Melasma: A Clinicopathological Study of 43 Cases. Indian J Pathol Microbiol. 2009.Jul-Sep;52(3):357-9. doi: 10.4103/0377-4929.54993. PMID: 19679960 [PubMed – indexed for MEDLINE]
15 Seçkin HY, Kalkan G, Baş Y, Akbaş A, Onder Y, Ozyurt H, Sahin M. Oxidative Stress Status in Patients with Melasma.Cutan Ocul Toxicol. 2013 Oct 22. [Epub ahead of print] PMID: 24147944 [PubMed – as supplied by publisher]
16 Strauss JS. Skin Care and Incidence of Skin Disease in Adolescence. Curr Med Res Opin. 1982;7(Suppl 2):33-45. PMID: 6213377 [PubMed – indexed for MEDLINE]
17 Verdier-Sévrain S, Bonté F, Gilchrest B. Biology of Estrogens in Skin: Implications for Skin Aging. Exp Dermatol. 2006.Feb;15(2):83-94. Review. PMID: 16433679 [PubMed – indexed for MEDLINE]
18 Wu IB, Lambert C, Lotti TM, Hercogová J, Sintim-Damoa A, Schwartz RA. Melasma. G Ital Dermatol Venereol. 2012. Aug;147(4):413-8. Review. PMID: 23007216 [PubMed – indexed for MEDLINE]
19 Zouboulis CC. Acne Vulgaris. The Role of Hormones. Hautarzt. 2010 Feb;61(2):107-8, 110-4. doi:10.1007/s00105-009-1830-1. German. PMID: 20107754 [PubMed – indexed for MEDLINE]


























0 Comments