
It seems that everyone wants to stay young; the quest for longevity is the number one goal of many individuals. Unfortunately, aging begins at birth and there is no magic potion to stop this natural process.
Externally, youthfulness is measured by looks, which is often equated with the skin’s appearance. People often judge a person’s age by the appearance of their face, noting wrinkles, sun spots, sagging, and the lack of a rosy pinkness and plumpness that is associated with youth. While others often reach these conclusions based on the outward appearance of the skin, what they see is often only a reflection of what is going on underneath. In other words, the true aging of the skin is taking place invisibly below the surface. Comprehension of skin aging requires an understanding of not only the visual changes but also the underlying physiological changes and how they correlate.
Controlling Skin Aging
Skin aging is constant and complex. Intrinsic aging and the physiological changes associated with it occur at a rate pre-determined by genetics and how it regulates the chronological aging processes. Extrinsic aging, due to external factors and various extents, can be controlled. These factors include exposure of the skin to the environment, lifestyle, and natural movement of the skin. Environmental factors include exposure to man-made pollutants, carcinogens (including nicotine), and ultraviolet radiation. At the same, time repetitive muscle movements associated with facial expressions also wear down the skin, particularly around the eyes and mouth. The effects of lifestyle represent the only truly-controllable environmental factor, including levels of sleep, diet, and overall health. It is not possible to separate intrinsic and extrinsic aging as they occur simultaneously. However, comparing areas on the body that have not been exposed to the environment, such as the torso, to areas that have been exposed, such as the face and hands, drastically demonstrates how well the skin can be preserved if it is only subject to intrinsic aging.
Well before visible changes occur to skin, aging is occurring beneath the skin at the tissue level (such as the movement of subcutaneous fat deposits) and microscopically, with changes to the biomolecular components of the skin beginning at the most basic level: skin cell DNA. DNA is the basic building block of chromosomes. Like other biomolecules in the body, it is subject to degradation and changes in its function. Aging of skin and other human tissues have been traced to molecular changes in chromosomes, specifically the unique molecules (telomeres) that protect DNA. As skin cells reproduce, a key requirement for the production of healthy skin, new copies of DNA are produced. However, while telomere protective proteins are also produced during the new daughter cell replication, they are shorter and less protective of the DNA. The shortening naturally continues during each successive daughter cell production and is a key part of intrinsic aging. Extrinsic aging factors, on the other hand, can also enhance telomere shortening. Shortening triggers inflammation, oxidation, and glycation. It can also lead to apoptosis, which can lead to cell death. Cell death, in turn, contributes to the aging process.
The molecular and physiological changes occurring deep within the skin can take years to produce the visible changes associated with aging. This delay is likely a large factor in why many people do not focus on skin health until much of the skin damage is well on its way. Skin aging starts to manifest itself as early as the teenage years. It may first appear as a permanent freckle or a faint expression line around the eyes. As each decade passes, subtle changes are noticed, which in later years tend to accelerate, changing both the appearance of the skin and the face shape as well.
The Twenties
During the 20s, skin is full of life and vigor. The epidermis is thick and the rate of cellular turnover is high. This rate of turnover stimulates new cellular proliferation, provides a healthy appearance to skin, and imparts great barrier protection and hydration. The production of ultraviolet-
protecting pigments in the epidermis occur at a normal level, providing protection to the skin against ultraviolet damage. Minimal, detectable sun damage is typically seen and a healthy glow presents a luminous complexion. Deeper within the skin, the dermis (which provides the key scaffolding and nutrition) is vibrant and functions normally. The key dermal proteins, collagen and elastin, are healthy and abundant, giving the skin excellent underlying support, fullness, and elasticity. The fibroblast cells within the dermis maintain production of these key skin proteins, as well as skin moisturizing factors. All of these components help to keep the formation of deep wrinkles in check.
A person’s 20s is the time where their lifestyle and daily preventative maintenance will determine how their skin will behave in later years; not smoking, reducing sun exposure or tanning, and using healthy doses of vitamins A, C, and E; alpha-lipoic; CoQ10; and green tea on the skin will protect both the epidermal and dermal skin cells from oxidative free radical damage. Using a non-
stripping, non-benzoyl peroxide exfoliating cleanser; a daily peptide moisturizer; an oil-free, chemical-free sunscreen; a high-dose antioxidant serum in the day; and a gentle exfoliating serum at night are all crucial steps that should not be skipped.

The most overt sign of skin aging begins in the late 20s and early 30s, principally with the appearance of facial wrinkles. As people proceed into this third decade of life, expression-line wrinkles or dynamic wrinkles are very common. Dynamic wrinkles form perpendicular to the long axis of facial muscles. Coarse wrinkles on the forehead, crow’s feet around the eyes, and laugh lines around the mouth begin to take shape as the skin can no longer bounce back after each muscle movement. These changes coincide with the thinning of the skin’s epidermis and dermis, as well as the subcutaneous fat-containing tissue. Furthermore, the quality of the skin’s proteins, collagen, and elastin start to deteriorate, which enhance fine lines, wrinkles, and skin dehydration. The thinning becomes most visible with the appearance of nasolabial folds.
Hormones also begin to play a great role in skin health. Estrogen levels peak, giving women the best skin ever. However, when these estrogen levels drop or are uneven, testosterone dominates and manifests itself in varying stages of acne.
A person may wake up one morning and notice that they still appear tired with sagging eyelids and under-eye bags. In these years, the eyebrows drop down and cause the intraorbital fat to bunch up and form bags. Sleep, diet, and skin maintenance can help alleviate this phenomenon. Many topical treatments (including peptides and histamine), like actives, provide excellent results in this area. The 30s is the time to start a serious age control regimen that includes strong retinoids, expression-line relaxing peptides, daily miniature peels, and internal hydration serums.
Hyperpigmentation
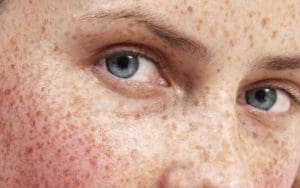
Skin discoloration also becomes more prominent during the 30s. Hyperpigmentation may be caused by hormones, ultraviolet exposure, and inflammation. Hormonal fluctuations during pregnancy and hormone-based medications, such oral contraceptives and hormone therapy, may contribute to the formation of melasma. The effects of ultraviolet exposure can further contribute to uneven skin tone; the damaging effects of this exposure are enhanced by changes in the distribution and production of eumelanin and pheomelanin, which provide ultraviolet protection and define skin color. Instrumental to protecting the skin against ultraviolet damage, the melanin pigments becomes scarcer during aging because the number of melanocytes in the epidermis decreases. Studies have shown that active melanocytes decrease with age at a rate of eight to 20 percent during each decade of life, diminishing the natural ultraviolet protection of the skin, which significantly contributes to the extrinsic aging process.
Until relatively recently, the traditional medical treatment for hyperpigmentation has been the application of topical products containing hydroquinone. However, hydroquinone has been called into question by various scientific studies pointing to its potential negative side effects. Skin care professionals are now moving towards safer, natural alternatives to combat all forms of hyperpigmentation, including (but not limited to) kojic acid, arbutin, soy, polyphenols, vitamin A, vitamin C, and glutathione. Depending on the type of hyperpigmentation present, there are various types of skin therapies. Epidermal pigmentation can be treated by either physically lifting the hyperpigmented epidermal cells with chemical peels or by stimulating cell turnover with retinoid treatments. These techniques can be combined with treatments to slow the natural pigmentation production, specifically melanin synthesis. Research has also focused on treating hyperpigmentation by inhibiting the formation of melanin by blocking tyrosinase. Tyrosinase is responsible for converting the amino acid tyrosine to a precursor of melanin. Another method of inhibiting melanin production involves the application of formulations that contain decoys, which effectively block the tyrosine-conversion process. Both methods reduce the concentration of melanin in the areas exhibiting hyperpigmentation.
Dermal pigmentation is significantly more difficult to treat. The pigmentation is deep within the skin and is, therefore, more challenging to treat, even with deeper-penetrating lasers. Any treatment of the dermis, whether chemical or laser, presents the risk of significant inflammation and potential scarring.
The presence of hyperpigmentation is often not an acute event. This occurrence progresses over time and, in aging skin, it appears in an area that will require continuous care.

If someone were to compare themselves in their 40s to a photograph from their 20s, they would not only notice wrinkles and skin color and texture changes, but also an overall change in their face shape. In the 40s, these changes occur in both the soft and hard tissues. Soft tissue changes include a loss of fat and a deterioration of facial muscle, leading to nasolabeal folds and the dropping of the cheeks and jowls. Furthermore, the skull begins to shrink and the nose bridge drops. Aging skin undergoes physiological changes as well, including structural and biochemical variations that lead to changes in permeability, barrier protection, water loss, cellular renewal, neurosensory perception, and some increases in certain skin diseases. It is informative to look at these progressive changes that start as early as the 30s and become more evident in the 40s and beyond.
Epidermal Aging
While changes in DNA set in motion intrinsic aging, the visible changes that are seen are a result of the changes in the cellular structure within the epidermis, such as the principal thinning and slowdown in the production of new cells and the degradation of key proteins in the dermis.
The epidermis sits on top of the dermis; these two layers have a synergistic relationship. The epidermis is a tightly-packed layer of cells (the top layer is packed with keratin protein) and provides physical protection to the dermis. It also resists the absorption of extraneous chemicals into the skin, absorbs damaging ultra violet radiation, and is the first line of protection against microbial invasion. The dermis contains a network of blood vessels that provide a source of nutrition and temperature regulation to the outlying epidermis. Nutrients are able to pass through the dermo-epidermal junction, the natural boundary between the two skin tissue types. The thicker dermal tissue provides the underlying scaffolding and padding with its dense matrix of fibrous, elastic, and water-binding proteins, specifically collagen, elastin, and glucosaminoglycans, respectively.
During the aging process, new cell growth and proliferation in the epidermis slows down as well. The once vital basal layer of the epidermis, which is responsible for producing keratinocytes, is less productive. The basal cells in the stratum basale consist of stem cells that are able to replicate through cell division and produce daughter cells. The new cells then begin a process of changing shape and function and eventually die off, producing a protective layer of dead cells on the outer surface. A key part of this desquamation involves the production of large quantities of keratin granules inside the cells most visibly seen in the stratum granulosum. These cells eventually die, leaving an envelope of the original cell packed with keratin. These protein packages provide a tough, protective outer surface to the epidermis, even though the layer is thin. As new cells are produced at the base of the epidermis, the outer cells of the stratum corneum slough off and create a fresher outer surface. 
To compound these changes within the epidermis, the delivery of nutrients from the dermis to the epidermis slows with age. This sluggishness may be due in part to changes in the dermo-epidermal junction. This junction consists of protrusions of dermal tissue into the epidermis. These finger-like insertions, called papilla, allow an intimate communication between the two layers. They are most pronounced in young skin and extend the border between the two layers, much like the interface between the surface of one’s hand and the inside of a glove. However, as people age, the papilla protrusions begin to decrease in size, leaving knob-like smaller intrusions. As a result, the overall communication between the layers is reduced. This reduction, in turn, decreases the surface area between the two skin layers and their intercommunication.
Professional Solutions
It is imperative to boost the renewal process of the epidermis with effective but controlled exfoliation methods, including chemical and non-chemical peels, physical scrubs, or dermabrasion and dermaplaning techniques. Everything in moderation applies perfectly to exfoliation and choosing the correct peel for the client’s skin type is imperative. These techniques should always be performed in conjunction with post-healing treatments that go beyond just applying a moisturizer. Incorporating antioxidants, peptides, healing vitamins, anti-inflammatory masks, and soothing moisturizers into both the professional treatment and a daily homecare regimen is key.
Dermal Aging
The dermis undergoes structural and biochemical changes with age, thinning and becoming less vital. This change is accompanied by a decrease in vascular blood flow and cellular replication. On a cellular level, the number of fibroblasts (the unique dermal cell responsible for producing the dermal proteins) reduces. The viable fibroblasts become less productive, leading to a reduction in the biosynthesis of the various skin collagens and the water-binding glycosaminoglycans. While production of elastin does not decrease, it does become irregular, thickening during the elastosis process and losing its snap-back properties. The reduction of collagen leads to a weakening of the key molecular scaffold in skin as the existing collagen matrix, which naturally oxidizes and deteriorates, is not replaced. As the skin is stretched and contracted, the instantaneous folds that appear in the skin become permanent as the skin is weakened by the loss in collagen rigidity and organization; the less flexible elastin is unable to quickly relax the skin to its original position. The permanent folds (such as deep wrinkles), are enhanced by a decrease in dermal hydration directly resulting from a reduction in glycosaminoglycans, principally hyaluronic acid. Hyaluronic acid and other glycosaminoglycans bind water and are the molecular component of the extracellular matrix.
Women’s skin sees this decline in dermal integrity faster than men. The loss of the estrogen hormone in women intensifies in the fourth and fifth decades due to the onset of menopause. Drastic differences in mechanical depression recovery are seen to bounce back within seconds in young skin when compared to hours in very old skin.
Subcutaneous Aging
The subcutaneous layer, also called the hypodermis, sits beneath the dermis and also undergoes changes with aging. The hypodermis is primarily made up of adipose tissue, blood vessels, and nerves. It is integral to cushioning the body, regulating body temperature, and binding the dermis to the underlying organs. Special connective tissue composed of collagen and elastin fibers attach the dermis to the hypodermis. While the volume decreases in the facial area and the hands and feet, it increases in the thighs, waist, and abdomen. The loss of fat leads to an increase in wrinkles and skin sagging, as well as less cushioning for the small blood vessels. With less protection, the small blood vessels tend to rupture and cause bruises. The impact of bruising is enhanced as the skin thins, becoming less opaque and more translucent. This occurrence also exposes telangiectasia.

Extrinsic Aging
Extrinsic factors play a major role in skin aging, with the most significant factor being ultraviolet radiation of the skin and its substructures. Penetration of damaging ultraviolet radiation has the effect of producing free radicals, particularly reactive oxygen species. These substances can quickly damage skin cell DNA, leading to potentially carcinogenic mutations, and collagen and elastin fibrils in the dermis. Reactive oxygen species free radicals can damage collagen fibrils in the skin by unraveling their structure or causing the fiber to fragment. In the case of elastin, ultraviolet exposure causes the fibers to thicken and cross-link, a process known as solar elastosis, harming the elastic function of the fibers. Ultraviolet radiation is also believed to enhance the formation of advanced glycation endproducts, which can be described as proteins and other biomolecules that become complex sugars. If elastin or collagen molecules are tagged with sugar molecules, their mechanical function is impaired. Unfortunately, ultraviolet-induced free radical damage is more difficult as the skin ages, demonstrating the effects that combining intrinsic and extrinsic processes have on skin health.
Menopause-Induced Aging
Unlike the high estrogen levels in the 20s that give the skin a beautiful, healthy, and hydrated glow, estrogen levels slow down to a halt, giving way to testosterone as menopause sets in. Almost one-third of collagen is lost within the first five years of menopause, further amplifying wrinkles, reducing facial volume, and taking away the plump, hydrated, glowing skin that only estrogen can give. Sebum production also slows down, reducing the overall lipid content by as much as 65 percent. Sebum provides emollience, lubrication, and a natural, thin film covering the skin’s surface. It provides a natural acid mantle coating against the skin, locking out harmful bacteria, yeasts, and molds. When combined with the loss of mucopolysaccharide production in the dermis, an increase in transepidermal water loss, and the reduction in the barrier properties of the epidermis, skin dehydration becomes both visible and palpable. Menopause also affects the circadian rhythms, disrupting the sleep patterns of women as they age. Sleeping is essential to cellular repair and the rejuvenation of key organs, including the skin. The role of inflammation also becomes more evident during this decade and beyond. The skin is now more susceptible to environmental factors, such as ultraviolet exposure, pollution, and lifestyle choices (like sleep, diet, and exercise).
The complexity of skin aging requires an integrated care plan that evolves over the years. It should include a daily homecare regimen with a professional clinical treatment plan. There is not a super ingredient or machine that will cure all of the skin’s aging woes. Instead, a steady, multi-faceted, individualized skin care plan is best. Progressive treatments, including acid and non-acid exfoliation methods, epidermal rejuvenating retinoids, epidermal youth supporting stem cells, dermal peptide messengers, and antioxidant-protecting vitamins, are key factors that should be included daily and used in skin care topicals. The anti-aging game is one where the methodical, steady, progressive approach always wins.
Skin care professionals can help clients address the signs of aging at both the dermis and epidermis by understanding the changes that occur to a targeted portion or function of the layer and the professional treatments that can be used to address those concerns.






















0 Comments