Hyperpigmentation is a prevalent skin disorder that has multiple causes and can be challenging to treat. Many people suffer through years of unsuccessful attempts at eliminating the disorder and may be reluctant to professional treatment. Understanding the underlying causes and predisposed factors with hyperpigmentation will help assess each situation and help prevent the onset of the disorder in some cases. The initial consultation and health history will help determine the exact cause of the disorder and help skin care professionals establish a successful treatment protocols for clients.
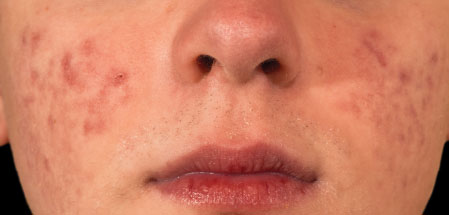 Post-Inflammatory Hyperpigmentation
Post-Inflammatory Hyperpigmentation
The process of inflammation that occurs in the body is a contributing factor to post-inflammatory hyperpigmentation. When treating inflamed acne or dark skin phototypes, reducing inflammation and inflammatory responses should be considered to reduce risk factors to post-inflammatory hyperpigmentation. Post-inflammatory hyperpigmentation is commonly found with acneic conditions, dark skin phototypes, and post-operative cosmetic procedures.
The inflammatory process occurs as a response to the body’s innate immune system and is the body’s attempt at self-protection from an injury or infection. When there is an injury to the skin, the body is alerted to the injured site. White blood cells called neutrophils are the first responders to an injury and will defend against small, inflammatory processes. Neutrophils decompose fragmented collagen at the site of the injury and trigger cells such as fibroblasts and macrophages to the wounded area. Macrophages play a crucial role in the inflammatory process by engulfing cellular debris as a response to repair tissue. The skin continues to go through this repair process, allowing growth factors, enzymes, and cytokines to produce granulated tissue until the area is healed. The inflammatory process removes harmful stimuli, damaged cells, irritants, and pathogens, which then begins the body’s natural healing process.
As a result to injury, various triggers include melanogenesis of the epidermal or dermal layers of the skin. Melanogenesis is the process in which melanocytes produce melanin. Melanocytes are cells that create the pigment found in the skin, eyes, and hair. Melanocytes produce melanosomes and comprise approximately 10 percent of the cells in the basal layer of the epidermis. Synthesis of melanin occurs exclusively in melanosomes from melanocyte activity. 
During the inflammatory process, a number of inflammatory mediators, including prostanoids, cytokines, chemokines, as well as reactive oxygen species, are released in the epidermal layer. Inflam-matory responses of the epidermal skin layer can alter the activity of im-mune cells and melanocytes, increasing production of melanin. In dermal melanogenesis, inflamma-tion disrupts the basal layer, causing melanin to be released and trapped in the macrophages of the papillary dermis, resulting in pigmentary incontinence.
The skin care professional should be aware of the two types of inflammation that can occur when treating skin conditions. Acute inflammation is short and can last from a few minutes to a few days. With acute inflammation, neutrophils predominate and usually occur with protein exudate. If left untreated, acute inflammation can continue and progress to chronic inflammation.
Chronic inflammation can last for days and occurs where tissue destruction is too massive to be resolved; it consists of infiltration of mononuclear cells, including macrophages, plasma cells, and lymphocytes. With chronic inflammation, tissue destruction can occur and result in post-inflammatory hyperpigmentation. When treating skin conditions, preventing chronic inflammation is a crucial post-operative cosmetic procedure.
Studies have shown that diet can contribute to inflammation in the body. When treating post-inflammator hyperpigmentation, the skin care professional can take a holistic approach by informing the client of benefits when eliminating white wheat and sugar from their diet. When treating lighter skin phototypes I and II, intense pulsed light (IPL) is the ideal treatment for post-inflammatory hyperpigmentation and can be combined with tyrosine inhibitors and chemical peels to improve the condition.
Ethnicity - A Predisposed Factor
When treating ethnicity, it is essential that the licensed professional have a thorough understanding of the inflammatory responses and the effects on ethnic skin. Racial ethnic groups such as Hispanic, Native American Indian, African, Asian, Middle-Eastern, and Eastern Indian are most prone to post-inflammatory hyperpigmentation. The difference between fair skin people and dark skin people is not due to the quantity of melanocytes, but to the size and level of activity of the melanocytes and the production of tyrosinase. Tyrosinase is an enzyme that is produced from the amino acid tyrosine and is required for melanocytes to produce melanin.
During the inflammatory process, melanocytes become hyperactive in darker skin phototypes, which can lead to post-inflammatory hyperpigmentation. The best way to prevent hyperpigmentation and post-inflammatory hyperpigmentation in darker, racial ethnicities is to have a proactive approach by preventing melanocyte stimulation. This can be done with topical ingredients that block tyrosinase and prevent melanocyte hyperactivity. Common ingredients that block tyrosinase include kojic acid, mandelic acid, thioctic acid, niacinamide, ferulic acid, and arbutin. Synergistic therapy includes tyrosinase inhibitors in combination with hydroxy acids such as mandelic acid or polyhydroxy acids. Another option for dark skin phototypes III to VI is prescription drugs that combine fluocinolone acetonide, hydroquinone, and tretinoin.
Melasma
A very common hyperpigmented skin disorder is melasma, also known as chloasma. Melasma appears as a tan or dark facial skin discoloration and is one of the most challenging skin conditions to treat. The skin care professional must understand that melasma can reappear. Symptoms of melasma include dark, irregular patches that are commonly found on the upper cheeks, nose, lips, upper lip, and forearms. These patches usually develop gradually over time. Melasma does not cause concern for any other symptoms beyond cosmetic discoloration.
Melasma is most prevalent in men and women of darker skin colors. The occurrence of melasma is commonly found in people of Native American Indian, German, Russian, Asian, or Jewish descent. When dealing with melasma, the skin care professional should consider both skin color and genetic predisposition. Ethnic factors should be considered with lighter skin phototypes, who could be genetically prone to melanocyte hyperactivity and hyperpigmented disorders. Women who have a light brown skin type and have had intense sun exposure are most susceptible to developing melasma.
Clients with darker skin types have a higher level of melanocyte activity and special care should be taken to prevent hyperpigmentation. Because of melanocyte hyperactivity, individuals such as African, Hispanic, Indian, and Asian with darker skin phototypes, Fitzpatrick type III to VI, are at greater risk of developing melasma and hyperpigmented disorders. 
When treating melasma, avoidance of ultraviolet radiation should be considered. Ultraviolet radiation contributes to the development and the exasperation of melasma and can cause both an increase in melanin production and transfer, as well as an increase in the number of melanocytes. Clients with lighter skin phototypes, Fitzpatrick type I to II, who live in an area of high sun exposure are at high risk of developing melasma.
Melasma is a condition that is commonly found in pregnant women, women taking oral contraceptives, or women on hormone replacement therapy (HRT). In pregnant women, melasma tends to fade post-partum, but can return with subsequent pregnancies. The discoloration will usually disappear over a period of several months after giving birth. On the other hand, melasma caused by oral contraceptive use typically does not fade after discontinuing use of the drug.
There are certain medical conditions that can bring the onset of melasma. The incidence of melasma increases in clients with thyroid disease and can also be associated with Addison’s disease, an endocrine disorder. With Addison’s disease, a minor injury can stimulate the onset of the melasma condition.
Other contributing factors to melasma may be the overproduction of the melanocyte stimulating hormone (MSH) brought on by stress. Other rare causes of melasma include aller-gic reaction to certain medications and cosmetics. Having a complete lifestyle and health history of the client can most often help determine the cause of melasma conditions.
Melasma is usually diagnosed visually or with a Wood’s lamp.  A Wood’s lamp is an ultraviolet lamp which shows hyperpigmentation and sun damage, and can determine if excessive melanin is located in the epidermis or in the dermis. When using a Wood’s lamp, the depth of the damage can be hard to determine. Most melasma is epidermal and can be treated with topical therapy, clinical procedures like chemical peels, and resurfacing procedures like microdermabrasion and laser peels. Dermal melasma can be more challenging to treat and can require medical procedures such as IPL or laser therapy.
A Wood’s lamp is an ultraviolet lamp which shows hyperpigmentation and sun damage, and can determine if excessive melanin is located in the epidermis or in the dermis. When using a Wood’s lamp, the depth of the damage can be hard to determine. Most melasma is epidermal and can be treated with topical therapy, clinical procedures like chemical peels, and resurfacing procedures like microdermabrasion and laser peels. Dermal melasma can be more challenging to treat and can require medical procedures such as IPL or laser therapy.
The best treatment for melasma is to avoid exposure to ultraviolet radiation. When preventing and treating melasma, the use of a broad spectrum UVA sunblock ingredient that contains zinc oxide is most preferred over the use of UVB chemical sunscreen blockers.
Sun Damage
Most sun damage occurs before the age of 18. Sun damage accumulates over time from chronic exposure to ultraviolet radiation and the results become prevalent with age.
Solar lentigines, also known as freckles, are light brown to black macules appearing on chronically sun-damaged skin. They are commonly found on the face, shoulders, neck, back, dorsal forearms, and hands. Lighter skin types are more affected by solar lentigines, but the condition can be found in all races and skin phototypes. Solar lentigines do not go away with reduced ultraviolet light exposure.
Chronic exposure to ultraviolet radiation is implicated as the cause of solar lentigines. With lentigines, there is an increase of melanin production and transfer to basal keratinocytes, as well as an increase in the number of melanocytes.
Other forms of sun damage include actinic keratosis, pre-cancerous skin cells caused from ultraviolet radiation exposure. Actinic keratosis appear as scaly, crusty lesions that form on the surface of the skin and can be light, dark, tan, pink, or red. The scale or crust is horned-like, dry, rough, and may disappear and reappear. They are usually not life-threatening, but it is important that actinic keratosis is diagnosed and treated early.  If actinic keratosis is suspected, it is best to refer the client to a medical doctor for proper diagnosis and treatment. Resurfacing procedures, such as medium and deep chemical peels, are commonly used to remove actinic keratosis and can be combined with IPL, laser resurfacing, or photodynamic therapy. Medically, topical prescription drugs or liquid nitrogen are used to remove pre-cancerous lesions.
If actinic keratosis is suspected, it is best to refer the client to a medical doctor for proper diagnosis and treatment. Resurfacing procedures, such as medium and deep chemical peels, are commonly used to remove actinic keratosis and can be combined with IPL, laser resurfacing, or photodynamic therapy. Medically, topical prescription drugs or liquid nitrogen are used to remove pre-cancerous lesions.
Other forms of sun damage include actinic bronzing and poikiloderma of civatte. With actinic bronzing, severe sun damage has occurred and the skin has an overall bronze appearance. Medium to deep chemical exfoliation can show dramatic results when treating actinic bronzing and can be combined with fractional laser therapy for optimal results. Conditions such as poikiloderma of civatte are a combination of both hyperpigmentation and vascularities. Ideally, IPL can be most effective to treat this condition.
When treating hyperpigmentation, the best therapy is a preventative approach, using topical antioxidants and daily use of a broad spectrum sunscreen. Knowing the client’s health history and predisposed factors of ethnicity will help determine the causes of the hyperpigmented disorder and determine the best treatment options. Having the client know and understand the causes of the hyperpigmented disorder will emphasize the importance of skin care and compliance to a treatment regimen.
 Linda Gulla is founder of the International Institute for the Advancement of Aesthetic Medicine, and offers advanced training to professionals as an educator and adjunct instructor in CME and CE. Gulla shares her knowledge in medical aesthetics, giving presentations to professionals at the International Dermal Institute. She has authored and published resource manuals in medical aesthetics and shared her expertise in advanced aesthetics as an editorial reviewer with Milady. Gulla provides professionals with opportunities for career advancement with the convenience of self-study, offering the first online certification in medical aesthetics, which includes content that has been accredited by the ACCME.
Linda Gulla is founder of the International Institute for the Advancement of Aesthetic Medicine, and offers advanced training to professionals as an educator and adjunct instructor in CME and CE. Gulla shares her knowledge in medical aesthetics, giving presentations to professionals at the International Dermal Institute. She has authored and published resource manuals in medical aesthetics and shared her expertise in advanced aesthetics as an editorial reviewer with Milady. Gulla provides professionals with opportunities for career advancement with the convenience of self-study, offering the first online certification in medical aesthetics, which includes content that has been accredited by the ACCME.
This email address is being protected from spambots. You need JavaScript enabled to view it.
Want to read more?
Subscribe to one of our monthly plans to continue reading this article.