
Caring for skin to eliminate dead corneocyte deposits from the stratum corneum (SC) epidermis to uncover a new generation of skin requires inherent biological desquamation and professional physical exfoliation functioning in concert. Several skin care and chemical manufacturers provide various professional products in the form of diverse constituents and instruments including, but not limited to, chemicals, enzymes, microdermabrasion, cavitation, benzoyl peroxide, acids, masks, mechanical beads, and other desquamating facilitators. It is important that skin care professionals know what the safest products are to use during exfoliation procedures.
There is an actual science to professional exfoliation.
Maintenance of the skin’s barrier function by epidermal metabolism holds that the SC is not dead, but actually possesses a limited form of metabolic activity. Equally important, the SC is a biosensor that signals the underlying epidermis to respond to external stressors, such as exfoliation in the form of peels, enzymes, mechanical stimulation, cavitation, and so on. The skin is sectioned off into three layers: epidermis, dermis and subcutaneous layer. The epidermis is the outer layer and is made up of four distinct cell types including the keratinocyte, melanocyte, Langerhans and Merkel cells. These cells travel in constant movement to the SC termination point until they no longer possess their nucleus and organelles, leading to their death.
The epidermis comprises a specialized stratified epithelium containing proliferating keratinocytes in the basal layer that exit the cell cycle, stratify and migrate through the suprabasal layers, ultimately giving rise to a cornified (corneocytes), dead cell layer in need of exfoliation.
The principal biological mission of the epidermis is to create the SC to protect the body from the outside world. Cell death awaits these epidermal keratinocytes. This crucial step results in the production of corneocytes. The terminally differentiated corneocytes that are shed from the skin surface are continuously replaced from underneath by keratinocytes. There is always a delicate balance between basal cell proliferation and shedding of corneocytes (desquamation) to maintain the constant thickness of the epidermis.
Interestingly, the SC is consistent tissue comprised of approximately 15 corneocyte non-neucleated layers and is approximately 75 percent of the epidermis volume. Every day, one new generation of a cell layer in the millions replaces the other (19,500,000 per square inch), materializing in the deeper SC, and the old layer of corneocytes flake off the skin’s exterior. During a lifetime, this shedding phenomena fills an area the size of about six football fields!
Your proficiency of skill begins with a thorough understanding of the epidermis physiology and its cell maturation.
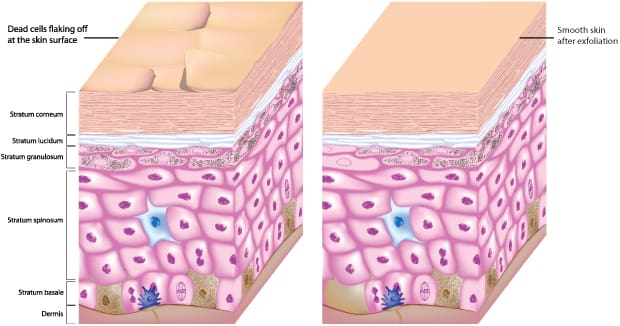
Keratinocytes are the main constituent of the epidermis and respond to a variety of inflammatory and immunomodulating cytokines, hormones, vitamins, ultraviolet light, toxins, physical, and controlled chemical injury. In its journey to the top layer of the skin, the keratinocyte goes through several transformations until it can act as a barrier cell. For example, the composition and size of cell – cell junctions, known as desmosomes – varies as keratinocytes progress through the upper epidermal layers. Constant formation and removal of desmosomes is required to allow the keratinocytes to move from the epidermal basal layer to the granular layer. Desmosomes are made up of complex proteins and are intercellular structures that link the intermediate filament cytoskeletal components between two cells and bond them together. These desmosome structures are extremely important to understanding exfoliation, given the desquamation process cannot proceed properly unless these desmosome bonds are broken to release the corneocytes.
Corneodesmosomes are modified desmosomes found in the SC, the uppermost layer of the epidermis. Here, they mediate strong intercellular cohesion to provide enough tensile strength to resist shearing forces that are crucial for the physical barrier function of the epidermis.
The skin’s natural cell turnover process is a complex series of steps that ultimately lead to the shedding of cornified dead skin cells, also known as a course of action called desquamation. Unlike the keratinocytes in the viable epidermis, the corneocytes of the SC are no longer able to synthesize new proteins, but enzymes, particularly transflutaminases, are involved in anabolic processes.
The role and function of the epidermal SC has two functions. One is a water-impermeable barrier function and the other is a buffer function against dryness. The water impermeability is due to the cellular lipid bilayer structure and the order of the corneocytes. The cornified envelope, which is formed on the surface of the corneocytes, plays an important role in the structure of the SC barrier affected by exfoliation.
The buffer function of the SC is due to water molecules in the corneocytes. Hydrophilic molecules such as amino acids hold water in the SC. Free amino acid content is a crucial factor, in that they contribute to the barrier function of healthy skin. Decrease of free amino acids in the corneocytes is characterized by dry, scaly skin and the decline of these functions leads to deterioration of the skin condition.
Skin turnover is a critical factor and plays a major role in the barrier function. The cells of the SC (corneocytes) result from the differentiation of the keratinocytes from the SC. The migration from this layer to the surface takes between 12 and 14 days, during which the cells differentiate and begin to die. The lifespan of the corneocytes in the SC is two to three weeks, as the superficial part of the SC is continuously desquamated at a balanced rate with the formation of new cells. For desquamation to occur, the cohesive corneodesmosomes binding the corneocytes in the SC must be degraded by enzymes, for example, proteases, which catalyses peptide bonds hydrolysis.
Building New Skin via Exfoliation
Inflammation results from a trauma and the response is seen in the blood vessels. The instant response of small capillaries in the area of injury is a vasoconstriction which lasts generally five to 10 minutes at the most, followed by active vasodilatation.
As stated previously, the epidermis is subject to constant wear and as a result, dead, horny cells of the outermost SC are constantly shed. Following a professional exfoliation, the corneocytes of the SC causes a trauma which causes the resting dermis to respond quickly to the shedding SC. This action results in the mechanism of regeneration called mitosis of preexisting cells. Mitosis occurs mainly in the cells of the basal layer and many of the daughter cells formed by cell division migrate into the upper layers of the stratum malpighi and, without further division, differentiate into keratinizing cells. The maximal increase in mitosis varies from 48 to 72 hours after injury. The main regenerative activity occurs in the basal cell layer and the dermis-epidermis junction is of considerable importance in healing of any trauma of the epidermis.
The dermis-epidermis junction is of a flat surface, but is defined by ridges known as rete ridges. It has been scientifically substantiated that alpha-hydroxy acids (AHAs) strengthen rete ridges worn by the aging process to help keep this junction intact. The portion of the dermis immediately under the basal cell layer consists of delicate collagenous elastic and reticular fibers, enmeshed with superficial capillaries and surrounded by viscous ground substance. Aestheticians know this dermal environment as the extracellular matrix (ECM) and professional exfoliation treatments are of great value to increase production of collagen, elastin, proteoglycans, hylauronic acid and other ground regulation substances to rebuild new skin.
It has been long recognized by the medical and science community that inflammation is necessary for skin repair.
Professional Alpha Hydroxy Acid Exfoliants
Alpha hydroxy acids (AHAs) are a group of organic acids that vary in the number of carbon molecules, and the information available on these much studied ingredients is endless. Hydroxy acids are organic carboxylic acids classified into A and B types (AHA, BHA) according to their molecular structure. Both AHAs and BHAs exhibit almost similar effects, however, AHAs are classified as a wounding agent and BHAs are recognized as non-wounding agent by the chemistry of their action on the skin. Chemical structure and natural source AHAs range from simple aliphatic compound to complex molecules. All have a hydroxyl group attached to the alpha carbon (the carbon adjacent to the acid group). The shortest-chain AHA is glycolic acid, which possesses two carbons, causing a rapid SC cascade of epidermolysis (a separation of the epidermal cells that can detach at the epidermal/dermal junction) and erythematic reaction. Lactic acid owns three carbons with less irritation, however, the benefits of this acid are substantiated and recommended as an effective tool for dry, acneic, and pigmented skin as it provides a natural moisturizing factor (NMF) comprised of 40 percent amino acids.
According to prominent scientist’s data on turnover and irritation, lactic acid’s long-term benefits increase firmness 35 percent, hydration 23 percent, smoothness 23 percent, wrinkles 55 percent, and collagen 210 percent. Lactic acid contains an NMF, which is known to hold onto water at the skin’s surface by binding hydration in place, signaling and assisting the skin proteins to better absorb moisture. NMF consists primarily of amino acids, a component of the important peptide chains and acid mantle. Given the differences of carbon structure and components of glycolic and lactic, these two related acid chemicals are the most commonly used AHAs in professional skin peeling and skin care formulas for anti-aging, rosacea, acne management and pigment control in retail end-user products. Other acids, also efficacious and used for skin peeling and skin care products, are identified by the terms: malic acid, citric acid, tartaric acids, alpha hydroxy (ethanoic, octanoic or caprylic) acid, pyruvic acid, trichlorocetic acid (TCA), retinol, mixed fruit acid, triple fruit acid, sugar cane extract, and any ingredient that includes the words alpha hydroxy, for example, tri-alpha hydroxy fruit acids.
The main principle of using acids on the skin is to remove surface proteins, mainly corneocytes. This is accomplished by denaturing the adhesive protein bonds (desmosomes) between these cells to cause a controlled injury by disrupting the acid mantle barrier. Proteins are complex biochemical compounds made of amino acids; the structure and function of a protein is determined by the sequence of amino acids that make up the protein.
A medical spin on this amazing ingredient substantiates that glycolic acid has been shown to be protective against UV-induced skin cancer, reduction of skin tumor incidence, a 55 percent reduction of tumor multiplicity, and a 47 percent decrease in the number of cancers larger than two millimeters. This inhibitory action is accompanied by a decreased expression of some UV-induced proteins such as proliferating cell nuclear antigen, cyclin D1, cyclin E, and cyclin dependent kinase 2 and 4 that regulate the cell cycle. These studied results medically suggest that glycolic acid may play an important inhibitory role on UV-induced tumor genesis.
Alpha hydroxy acids have no known systemic toxicity and are also classified as antioxidants that scavenge free radicals. It has been reported that these acid constituents can actually boost the skin’s sun protection factor
(SPF) capability.
Alpha hydroxy acids should be the most important ingredient of professional exfoliation treatment options. These chemical peels provide drastic results for managing photo-damaged skin and are more effective than microdermabrasion – erasing fine lines and giving the skin an instantaneously plumper, hydrated and smoother appearance with one to three applications. These state-of-the-art treatments must be repeated every three to six months in order to maintain healthy skin. In addition to the obvious cosmetic results of smooth and younger-looking skin, AHAs also stimulate the production of collagen and elastin and are reported to improve wrinkling, roughness and mottled pigmentation of photodamaged skin.
These miracle acids have been studied thoroughly and extensively and have been scientifically substantiated to:
- Decrease SC cohesiveness
- Increase thickness of viable epidermis
- Increases deposition of hylauronic acid (HA)
- Induce reversal of basal cell atypia
- Increase restoration of rete ridges
- Increase secretion of lamellar bodies (fundamental for barrier function of the SC)
- Reduce corneocyte cohesion by influencing bonds

30 Percent Protease: The New Advanced Exfoliation
Protease interest in skin arose with the realization of the important role of proteolysis in many biological phenomena. Early research of Sexsmith and Petersen in 1918 showed that there is considerable proteolytic activity in human skin. Since then, huge efforts have been made to characterize the pattern of the proteolytic enzymes and the pathways of proteolysis in normal and pathological skin.
Proteases have a specific role in orderly desquamation of the SC. Skin researchers have great interest in this specialized ingredient, because it possesses the process which regulates the condition of the skin. These safe and amazing cellular desquamating enzymes break down desmosomes one by one, releasing the hold on these structures, revealing new skin.
The SC has a depth-dependent dynamic structure in which multiple enzymatic reactions are balanced to ensure that mechanistic, cohesive and desquamatory properties are maintained. Proteases play important roles in the keratinization process but are also involved in tissue remodeling, lipid barrier homeostasis, and inflammatory conditions.
A non-injury exfoliation procedure that relies on biological action rather than physical abrasion (microdermabrasion) or wounding agents, the protease peel mimics Cathepsin D (the skin’s natural enzyme that controls exfoliation and cellular turnover). The body produces various proteolytic enzymes that include Cathepsin D to digest non-neucleated cells after death. This high-tech ingredient is gentle, self-neutralizing, and can be used on the most sensitive of skins, increasing skin penetration of other topical ingredients. Extremely safe, protease makes it the perfect exfoliation treatment solution for all skin types, skin genders, and skin of color.
The phenomena of a 30 percent acid protease exfoliation peel is that it works on one cell at a time, releasing the desmosomes and corneodesmosomes to induce the shedding of the squames at the outer layer of the epidermis at a rate that is uniquely balanced by mitotic development of new cells at the basal layer.
Proteases induce the shedding of scales (also known as flakes) of the SC corneocytes at a rate that is balanced by the mitotic development of the new basal cells. In other words, protease exfoliation works naturally with the skin’s biochemistry, allowing a balance between cell shedding at the surface of the epidermis and the proliferation in the basal layer of the epidermis, which is necessary for the formation of a normal stratum corneum.
Although protease is categorized as a peel because it possesses the mechanical action of an AHA without the wounding action, there is no visible flaking due to its digestive action of the non-neucleated cells. It penetrates into the stratum spinosum, releasing the desmosomes one at a time, allowing for greater desquamation without the injury.
In conclusion, desquamation and exfoliation is of crucial importance for the maintenance and overall function of the SC for an ageless appearance and healthy skin. A balance between cell shedding at the surface of the epidermis and the proliferation in the basal layer of the epidermis is necessary for the formation of a normal SC to assure a physiochemical barrier against a hostile environment and prevent water loss of this organism. The desquamation/exfoliation process is a precisely controlled cascade of events. Knowledge about the SC cell cohesion and the role of protease has evolved and more information involving this miracle enzyme in desquamation regulation has developed, providing the aesthetic industry an exciting new treatment tool for exfoliation. Further research of the SC and other exfoliation products is ongoing and is expected to give important contributions to this important area of aesthetic skin biology.






















0 Comments