
In our aesthetic culture today, the word ‘cellulite’ has come to represent a hideous fat condition of the human body where by we will do just about anything to rid it. The term was first used in the 1920s and began appearing in English language publications around the late 1960s. The earliest reference appeared in Vogue magazine, the prestigious fashion journal. Vogue introduced this new word for ‘fat’ into American society and from then on, controversy has surrounded cellulite for decades whereby medical doctors, scientists, and other professionals cannot agree if this foundation of fat really exists. Many doctors have flatly refused to acknowledge the existence of cellulite and still do despite the overwhelming scientific evidence.
Given that, among the believers there still remain strong opinions that debate the condition, cause, treatment and management of cellulite. And because of the ‘cellulite controversy,’ the last nine decades has spawned a wide range of clinical and home care remedies that have in part been loosely based on solid research and antidotal data used to market these products.
Over the last several months, I have reviewed numerous studies as my sources for this educational editorial and whether you agree or disagree, my intent is to help tear down this controversy and present solid science to facilitate the right products and cellulite treatment for a successful end point result.
What is this fat called Cellulite?
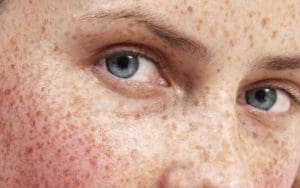
Cellulite has been established as a common body fat condition occurring in women (and to a lesser extent, men) that consists of inflammatory adipose material known as one of a constellation of connective tissue disorders (CTD) with still unidentified, related causes. This unsightly skin condition is generally referred to as “cottage cheese” or “orange peel” skin and is visibly detected in the abdomen, thighs, pelvic region, and arms. Given this, it is believed by many in the scientific community that the only “true” cellulite occurs in the buttocks and thighs. These regions of fat deposit still remain another debate with the medical community and will be addressed in this editorial.
Cellulite is not related to overweight body mass; it can affect both average and underweight individuals. Because of this fact, weight loss and cellulite management are two separate issues, making this unattractive superficial fat the last to be affected by exercise and diet. Although doctors recommend a health conscious pattern of eating as a cellulite antidote, the reality is this approach does not rid the ugly fat, only facilitates prevention and the formation of excess adipose tissue in the body that later can turn into inflammatory material. This approach is used as a preventative and not a cure to the condition. Diet is only one resolution of many for cellulite management.
Cellulite is a nasty, particular form of fat trapped between water located just below the dermis that builds and begins to form ugly bumps and bulges through the skin, effecting 90 percent of women. Why are women more predisposed to cellulite than men? One reason is women organize fat parallel to their skin causing a pulling-down effect making this physiological consequence primarily responsible for the bulges in the skin. In addition, hormones, predominantly Estrogen, play a central role in the formation of cellulite. Estrogen appears to initiate and aggravate this fatty substance.

Many myths and false information surround this “dreaded dimple disease” that has led to a booming and profitable cellulite industry primarily focused on the hope of the sufferer to rid the condition. However, the science points to predisposing genetic factors such as gender, race, biotype, a hormone allele determining the receptor number and sensitivity, distribution of subcutaneous fat, and predisposition to circulatory insufficiency. Although the aforementioned are not necessarily the total cause and factor of cellulite, these manifestations have been linked to their role as primary ‘aggravating sources.’ Most cellulite ‘cures,’ by which doctors and scientists agree, have been ineffective. Recent research points to the ‘real substance’ of cellulite that actually are the product of anatomy, genes, and hormones.
Very few men are affected with cellulite. Aside from the hormone connection, one reason could be based on the composition and conduct of women’s fat cells and the connective tissue that holds them in place. Simply put, a woman’s connective tissue is inflexible therefore as females gain weight the fat cells expand, bulging upward towards the surface of the skin creating the ‘orange peel/cottage cheese’ appearance. In men, the outer skin is thicker coupled with less fat on the thighs obscuring the physiological event occurring just below the surface.

The Hormone Cellulite Influence
Hormones control over 300 of our body’s responses and cellulite is a target for these commandos. Although Estrogen plays a dominant and significant role, other hormones such as insulin, the catecholamine adrenaline, noradrenaline, thyroid hormones, and prolactin have all been shown to have influence in the development of cellulite.
It is common for pubescent females as young as 11 to display some degree of cellulite, thereby connecting the ‘dots’ to the hormonal component and its unwelcome ‘orange peel’ skin appearance. Cellulite is rarely seen in males but common with those men who have androgen-deficient conditions such as Klinefelter’s Syndrome, hypo-gonadism, and males receiving estrogen therapy in the event of some prostrate cancers. The cellulite becomes more severe as the androgen deficiency drops in these males, lending credibility to the estrogen hormone connection. Testosterone, the male hormone, or some modification of this hormone, is being considered as a potential therapeutic agent in estrogen driven disorders such as cellulite. Be that as it may, still little science supports the totality of comprehensive cellulite understanding and although this fatty syndrome afflicts primarily women, it also appears to bypass Asian females… leaving the question: why do some women get cellulite and others do not?
What we do know, is recent conclusive studies site that cellulite appears to occur in certain families leaving many questions to be answered. What could be the hereditary component? Is there a preventative gene, or an absent gene in the cellulite-free women? A retrospective study found genetic factors such as personal history; family history and race were the most significant predictors for the striae maturity.
One recent study, (Chang et al, 2004) asserts striae, pelvic relaxation, and varicose veins appear to be related to the action of matrix metalloproteases’ (MMP) activity initiated by estrogen and that the physical manifestations of cellulite are due to destruction of the normal architecture of collagen trabeculations that keep the adipose tissue confined to the deep and superficial fat layers. (Lockwood, 1991)

Estrogen stimulates fibroblasts in connective tissue to produce MMPs degrading the collagen fibers that make up the trabeculations in the adipose tissue. Collagenase in connective tissue destruction is partly responsible for the local spread of cancer and metastases. We know that fibroblasts in the ECM (extra cellular matrix) represent a heterogeneous population of these active cells (Sorrell and Caplan, 2004), but we know little about what controls fibroblast cell functions (Haczynski et al, 2002, Hudelist et al, 2005, Chen et al, 2003, Kokorine et al, 1997, Sorrell and Caplan, 2004).
The role of the ECM (extracellular matrix) is not fully identified in connective tissue disorders. The ECM contains structural proteins that interact with integrins on the surface of the fibroblasts, which appear capable of directing the production of either collagen or collagenase via the direction of the mechanical forces exerted on the integrins. The role of integrins in health and disease is currently a vast area for skin research.
There appears to be an inverse dose dependent relationship between the level of estradiol and the proliferation of ACL fibroblasts (anterior cruciate ligament). Fluctuation in estrogen levels have been shown to be associated with ACL injury and these disorders appear to be the result of either the direct action of estrogen on connective tissue proteins or an indirect action of estrogen mediation through fibroblasts.
Cellulite in females begins with puberty and progresses throughout their life span. After menopause, the fatty tissue stroma supplies the estrogen via conversion of adrenal androstendione to estrone by the enzyme aromatase. Cellulite is a prototypical progressive estrogen-MMP connective tissue disorder (CTD), perpetuated by the rise and fall of menstrual hormones. The major target tissue in the uterus for both estrogen and MMPs is the endometrium, which consists mainly of collagen.
The build up and destruction of the edometrium each month during menses is a complex process orchestrated by the ebb and flow of estrogen and progesterone, which drives several different MMPs, particularly MMP 1, MMP 3, MMP 7 and MMP 9. Stromal collagen Type-1 appears to be the major target in cellulite, not the adipocytes. Prior to the appearance of ‘true cellulite,’ pendant tissue is attacked first, mainly the buttocks and the breasts. In addition to the MMP destruction, the constant gravitational force and immature biped anatomy provides no real support for these heavy structures.
Based on the aforementioned, the ‘true cellulite’ area is cited as the buttocks and thighs by scientists. Differentiation is identified by the adipocytes in this area that contain a greater number of adrenergic receptors (anti-lipolytic) than adrenergic receptors (lipolytic). These receptors account for the resistance of adipose tissue mobilization in these two anatomical sites.
The physical manifestations of cellulite are due to damage of the normal architecture of the collagen trabeculations that keep the adipose tissue confined to just two layers – the deep and the superficial layers.
What is the conclusive science connecting hormones and cellulite that we as licensed skin care professionals must understand of this condition? The answer is that cellulite is a connective tissue disorder resulting from the action of estrogen on fibroblasts to produce MMPs that damages connective tissues. This process is driven by the reproductive action causing sex hormone levels to surge. The majority of CTD in females are related to this process and scientists have been aware of the MMP action for years only recently making the critical cellulite connection.
Lifestyle, Underpants, and Cellulite
To a lesser extent, lifestyle plays a contributing role to cellulite. It has been written that the way we live is really the ultimate irritating cause of cellulite and their contributing factors that continue the controversy.
Tension, fatigue, poor eating habits, smoking, fatty and starchy foods, insufficient water intake, poor breathing, sedentary living, lack of exercise, polluted air resulting in sluggish digestion, constipation, poor circulation, standing, sitting or restriction of movement for long periods of time have all been connected to the increase of cellulite. I call it life.
It is also suspected that a high stress lifestyle is linked with cellulite because an increase of the catecholamine hormone is released into the blood stream causing imbalance of the system that ultimately activates free radical activity, exacerbating inflammation within the connective tissue.
Just when you thought it could not get any worse, it appears that our preference to what type of underwear we choose can also intensify cellulite. According to several credible references, wearing tight under garments limits blood flow to the body, triggering additional cellulite to form. Not the best news in a ‘under garment control’ fashion world. They give us a solution for hiding unsightly bulges only for us to discover these tight clothes could affect cellulite adversely. But there is a light under those tight garments; I understand there is a development in anti-cellulite panty hose to help combat the ‘cottage cheese’ that increases the blood flow to reverse the condition. I say, bring that on! The sooner the better.
Cellulite Classification
Cellulite is graded in three specific categories to determine what type of condition is present. Treatment should be rendered accordingly.

Cellulite Therapy
Now that we have a comprehensive understanding of the cause and effect of cellulite, we must turn to the immediate and long-term solutions to manage this condition. Numerous therapies have been developed and initiated to control cellulite. Unfortunately, with the buffet of different remedies available via retail, professional, and medical means, there are no published reports in the scientific literature substantiating that any of these modalities work to rid the condition. Manage cellulite, yes; eradicate cellulite, no. Having established this fact, it is the responsibility of the licensed aesthetic professional to provide a ‘management system’ for a cellulite condition and do further research on the many modalities available to ensure the remedy you select is compatible for the condition and grade of the cellulite to be treated. Keep in mind; it will require more than one remedy to achieve management success.
Some of the more popular physical, mechanical, and product methods to treat cellulite are: Iontophoresis; ultrasound; thermotherapy; pressotherapy (pneumatic massaging in the direction of the circulation); lymphatic drainage (gentle massage to stimulate lymphatic flow and reduce tissue inflammation); electrolipophoresis (application of a low frequency electric current); creams and gels that contain pharmaceutical and cosmetic agents such as mexthyxanthines (theobromine, theophylline, aminophylline, caffeine) which act through phosphodiesterase inhibition, and pentoxifylline that improves microcirculation; the adrenergic beta-agonists isoproterenol and adrenaline; the adrenergic alpha-antagonists yohimbine, piperoxan, phentolamine, and dihydroergotamine; the methylxanthine enhancers Coenzyme A and the amino acid l-carnitine; the drugs with connective tissue activity sillicium and Asiatic centella; and the microcirculation active drugs Indian chestnut, gingko biloba, and rutin in different combinations and application methods.
Given all the expensive and experimental treatment options via aesthetic mechanical and medical means, there still remains an alternative choice with the application of daily cellulite creams and lotions. Many formulas have a solid history in achieving results because these products are used daily and have been developed to target cellulite. These formulas produce temporary results, therefore must be used every day to be effective in controlling cellulite. Specialized cellulite creams and lotions can have a significant and dramatic effect when directions are followed specifically. Adipose tissue can be reduced with specific lypolytic agents and the best products contain ingredients to target the cellulite tissue to help reverse the ‘orange peel’ condition.
In conclusion, cellulite is never cured, only supervised with a careful selection of treatment. This ‘dimple disease’ requires a continued healthy diet, exercise, massage, and proven products by which this genetically predisposed, hormone driven fat condition is controlled and managed for effective endpoint results.

An inducted Legend in American Aesthetics by DERMASCOPE Magazine and Aesthetics International Association (AIA) in 2008, Christine Heathman has been a practicing licensed master aesthetician, educator, and a leader in the research and development of skin care and progressive clinical protocols for over 25 years. A recent testimonial to Heathman’s skin knowledge selected her amazing product formulas out of thousands and recently featured them on the nationally syndicated TV show called The Doctors, as an alternative option to cosmetic surgery. www.glymedplus.com




















0 Comments