Menopause is a major biological transition that extends far beyond the reproductive system. For many women, skin becomes one of the most visibly affected organs during this stage of life. Declining estrogen levels influence barrier integrity, inflammation, vascular reactivity, sebaceous activity, and melanocyte function – creating a perfect storm for acne, rosacea, and hyperpigmentation to emerge or worsen.1 For skin care providers, understanding the unique dermatologic shifts that occur during menopause is essential for delivering effective, compassionate, and results-driven care.
THE ESTROGEN EFFECT
Estrogen plays a critical role in supporting skin thickness, hydration, collagen synthesis, and immune balance. Estrogen receptors found throughout the epidermis and dermis, influence fibroblast activity, lipid production, and wound healing. As estrogen declines during perimenopause and menopause, skin undergoes several structural and functional changes, including reduced collagen production, increased transepidermal water loss (TEWL), slowerepidermal turnover, and heightened inflammatory responses.1,2 These changes increase skin sensitivity and lower tolerance for aggressive treatments, which is particularly relevant when managing inflammatory skin conditions in menopausal clients.
A DIFFERENT KIND OF FLARE UP
Although acne is commonly associated with adolescence, it often persists or newly develops during perimenopause and menopause. Declining estrogen levels combined with relatively stable androgen activity can lead to an increased androgen-to-estrogen ratio, stimulating sebaceous glands and contributing to follicular obstruction.3 Menopausal acne typically presents along the lower face, jawline, and chin and may be accompanied by increased dryness and sensitivity due to impaired barrier function.3,4
PROFESSIONAL MANAGEMENT
Effective acne management in menopausal skin requires a balance between treatment efficacy and barrier preservation. Evidence supports the use of low-dose topical retinoids, such as adapalene or tretinoin, to promote cellular turnover and reduce comedone formation while also addressing post-inflammatory hyperpigmentation (PIH).4
Salicylic acid may be helpful for follicular decongestion but should be applied conservatively to avoid worsening dryness. Barrier-repair moisturizers and gentle cleansers are essential components of any acne treatment plan for mature skin. In-spa treatments, including mild chemical peels and light-based therapies, can be beneficial when individualized to the client’s skin tolerance.⁵
ON ROSACEA
Rosacea is a chronic inflammatory condition characterized by facial erythema, flushing, telangiectasias, and inflammatory papules or pustules. During menopause, vasomotor instability and increased skin sensitivity may intensify rosacea symptoms, particularly flushing episodes. Hot flashes themselves can act as a trigger for rosacea flares.⁶
While epidemiological studies suggest that the overall incidence of rosacea may decline after menopause, the use of menopausal hormone replacement therapies have been associated with an increased risk of rosacea, highlighting the complex relationship between exogenous hormones and inflammatory skin responses.⁷
Evidence-Based Treatments
First-line rosacea management focuses on inflammation control and trigger avoidance. topical agents such as metronidazole, azelaic acid, and ivermectin are known in the literature for reducing inflammatory lesions while preserving barrier function.⁸
For moderate inflammatory rosacea, low-dose oral doxycycline is often prescribed to patients for its anti-inflammatory effects. Laser and light-based therapies, including intense pulsed light (IPL), are effective adjuncts for persistent erythema and telangiectasia.⁸ Lifestyle counseling – particularly around heat exposure, alcohol, spicy foods, and emotional stress – is an essential part of long-term management.⁶
MELANIN IN MOTION
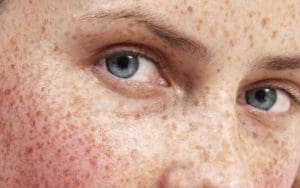
Estrogen plays a regulatory role in melanocyte activity and melanin distribution. As estrogen levels decline, pigment regulation may become inconsistent, particularly in skin with cumulative ultraviolet exposure. While classic melasma is more common during reproductive years, post-menopausal hyperpigmentation and extrafacial melasma are also prominent, as it is known to affect menopausal women in the fifth decade of life.9, 10, 12 Moreover, this condition shares similar clinical features as that of facial melasma with brownish hyperpigmented spots and irregular borders.12 Inflammation from acne or rosacea may further contribute to post-inflammatory hyperpigmentation, especially in skin of color.
Management & Prevention
Sun protection is still the cornerstone of hyperpigmentation management. Daily use of broad-spectrum sunscreen has been shown to prevent worsening pigmentation and improve treatment outcomes².
Topical agents such as hydroquinone, tranexamic acid, and retinoids help reduce existing pigmentation and prevent recurrence. Professional treatments, including chemical peels and laser therapies, may be considered for resistant cases, but must be approached cautiously due to increased sensitivity and slower healing in menopausal skin.¹¹
IN THE TREATMENT ROOM
Skin care providers play a critical role in guiding menopausal clients through skin changes that are often unexpected and emotionally distressing. Best practices include prioritizing barrier repair, avoiding overly aggressive protocols, reinforcing consistent homecare routines, and collaborating with dermatology or integrative health providers when necessary.² Menopause is a physiological transition – not a skin care failure – and it requires a compassionate, informed approach.
PROVIDER-LED SUPPORT
Acne, rosacea, and hyperpigmentation during menopause reflect interconnected hormonal, inflammatory, and barrier-related changes in skin. By understanding the underlying mechanisms and applying evidence-based strategies, skin care providers can help menopausal patients achieve healthier, more resilient skin while supporting confidence and quality of life during this transformative stage.
References
- Thornton, M. J. (2013). Estrogens and aging skin. Dermato-endocrinology, 5(2), 264-270. American Academy of Dermatology Association. (2023, November 20). Caring for your skin in menopause. American Academy of Dermatology Association. https://www.aad.org/public/everyday-care/skin-care-secrets/anti-aging/skin-care-during-menopause
- Harper, J. C., LF, S. G., Alexis, A. F., & Tan, J. K. (2018, June). Treating Acne in Adult Women. In Seminars in cutaneous medicine and surgery (Vol. 37, No. 3S, pp. S67-S70).
- Zaenglein, A. L., Pathy, A. L., Schlosser, B. J., Alikhan, A., Baldwin, H. E., Berson, D. S., … & Bhushan, R. (2016). Guidelines of care for the management of acne vulgaris. Journal of the American academy of dermatology, 74(5), 945-973.
- Castillo, D. E., & Keri, J. E. (2018). Chemical peels in the treatment of acne: patient selection and perspectives. Clinical, cosmetic and investigational dermatology, 365-372.
- Two, A. M., Wu, W., Gallo, R. L., & Hata, T. R. (2015). Rosacea: part II. Topical and systemic therapies in the treatment of rosacea. Journal of the American Academy of Dermatology, 72(5), 761-770.
- Wu, W. H., Geng, H., Cho, E., Eliassen, A. H., Drucker, A. M., Li, T. Y., … & Li, W. Q. (2022). Reproductive and hormonal factors and risk of incident rosacea among US White women. Journal of the American Academy of Dermatology, 87(1), 138-140.
- Thiboutot, D., Anderson, R., Cook-Bolden, F., Draelos, Z., Gallo, R. L., Granstein, R. D., … & Tan, J. (2020). Standard management options for rosacea: the 2019 update by the National Rosacea Society Expert Committee. Journal of the American Academy of Dermatology, 82(6), 1501-1510.
- Zhang, J., Wang, T., Li, Z., Qin, C., Dai, J., Zhao, Y., … & Jia, Z. (2025). Hormonal Crosstalk in Melasma: Unraveling the Dual Roles of Estrogen and Progesterone in Melanogenesis. International Journal of Molecular Sciences, 26(22), 10856
- Snyder, A., Schiechert, R. A., & Zaiac, M. N. (2017). Melasma associated with topical estrogen cream. The Journal of clinical and aesthetic dermatology, 10(2), 57.
- Grimes, P. E. (2009, June). Management of hyperpigmentation in darker racial ethnic groups. In Seminars in cutaneous medicine and surgery (Vol. 28, No. 2, pp. 77-85). WB Saunders.
- Madke, B., Kar, S., Yadav, N., & Bonde, P. (2016). Extrafacial melasma over forearms. Indian dermatology online journal, 7(4), 344–345. https://doi.org/10.4103/2229-5178.185470
Dr. Zakiya M. Cush, MSTOM MPH is board-certified by the NCCAOM and specializes in cosmetic acupuncture & holistic dermatology. Dr. Cush implements Traditional Chinese Medicine and Chinese herbalism therapies to help refine the way the skin ages, thereby creating a healthy and radiant glow from the inside out. Dr. Cush is committed to educating healthcare providers and the public on dermatologic health issues related to skin of color. Sheis a certified integrative microneedling practitioner, certified aesthetic laser technician, and she successfully completed the first nationally recognized 100-hour Advanced Cosmetic Facial Acupuncture program, taught by the esteemed Dr. Shellie Goldstein, L.Ac.



































0 Comments