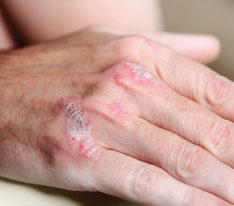
Some skin diseases are more than skin deep. Psoriasis is the most prevalent autoimmune disease in the country, affecting as many as 7.5 million Americans. This non-contagious condition often appears on the skin as red, scaly patches that itch and bleed. Psoriasis frequently starts between the ages of 15 and 35, but can appear at any time. New research indicates that chronic inflammatory conditions such as psoriasis may actually cause HDL cholesterol to change its molecular composition and increase the risk of severe heart disease. It is my opinion that the reasons to treat psoriasis are more important now than ever.
And because there are so many different medications for the condition, it takes experience and patience for the right treatment or combination of treatments to be successful.
As of now, psoriasis is incurable; however, treatments ranging from topical to systemic can treat it and often clear the symptoms. Psoriasis is marked by an overactive immune system that speeds up the growth cycle of the skin. In normal skin, new cells surface about once a month, but with psoriasis, new cells full with inflammatory cells surface in just three to seven days. Due to this rapid turnover, these cells build up into thick patches that have a silvery, flaking crust. Stress is a common trigger of psoriasis, along with diet, medications, cuts, scrapes, infections and allergies. According to findings presented at the summer 2011 meeting of the American Academy of Dermatology, when psoriasis patients feel stressed about their condition, it can aggravate their symptoms and impact their emotional state, which becomes a vicious cycle adding to their stress. Doctors previously thought that chemicals released by the skin's nerve endings only stayed in the skin when they were released. But doctors now understand that those chemicals travel to the brain and deplete the chemicals that regulate our emotions, such as serotonin, norepinephrine and dopamine.
Treating Psoriasis
Topical Treatments – Usually the first kind of medicine dermatologists use to treat psoriasis. These creams can slow the growth of skin cells and decrease the inflammation of skin lesions.
Phototherapy or Light Therapy – Usually involves consistent exposure to ultraviolet light at a doctor's office or with the sun. It is often used on patients with extensive psoriasis, moderate to severe psoriasis and combined with topical treatments. There are two different kinds of light therapy that utilize either UVA or UVB light.
Ultraviolet Light B (UVB)/Ultraviolet Light A (UVA) Treatments – Present in sunlight, UVB is an effective treatment for psoriasis because it penetrates the skin and slows the growth of affected skin cells. Treatment involves exposing the skin to an artificial UVB light source for a set length of time on a regular schedule at a doctor's office. There are two types of UVB treatment, broad band and narrow band. The narrow band UVB releases a smaller range of ultraviolet light. Many studies indicate that narrow-band UVB clears psoriasis faster and produces longer remissions than broad-band UVB.
Laser Treatments – Delivers a single high intensity narrow beam of ultraviolet light of 308 nanometers to target specific smaller areas of skin lesions. It works faster than either the UVB or UVA. It also only treats the affected skin sparing normal skin from side effects. There is no pain or bruising. Patients usually receive two treatments per week until clear.
 Pulsed Dye Laser – Uses a dye and different wavelength of light than other UVB-based treatments, pulsed dye lasers destroy the tiny blood vessels that contribute to the formation of psoriasis lesions. Treatment consists of 15 to 30 minute sessions every three to four weeks and it usually takes two to six sessions to clear the target lesion. It unfortunately has bruising and there is
Pulsed Dye Laser – Uses a dye and different wavelength of light than other UVB-based treatments, pulsed dye lasers destroy the tiny blood vessels that contribute to the formation of psoriasis lesions. Treatment consists of 15 to 30 minute sessions every three to four weeks and it usually takes two to six sessions to clear the target lesion. It unfortunately has bruising and there is
some discomfort.
Systemic Treatments – Prescription drugs given in the form of a pill or an injection. Because of their potential risks, systemic treatments are mostly used to treat more severe cases of psoriasis which have failed the moderate treatments listed above.
Biologics Biologics – Systemic treatments made from proteins produced by living cells. They block parts of the immune-system process that drives psoriasis. Scientists are excited about a new biologic that may even keep psoriasis at bay: The October 2011 issue of the New England Journal of Medicine chronicles a study wherein German researchers administered an experimental treatment of briakinumab, or a commonly used drug, methotrexate. Briakinumab stems an overactive immune system by blocking two proteins that drive inflammation. This experimental drug reduced psoriasis symptoms by 75 percent in more than 80 percent of the study participants, compared with only 40 percent of people who took methotrexate a long time accepted treatment for psoriasis. After a year follow-up, nearly 60 percent of participants taking briakinumab had no skin lesions, compared with fewer than 20 percent of participants taking methotrexate.
Patients today have many options for treating psorosis. I encourage people to talk with their dermatologist to determine the best course of action for their specific case.
Want to read more?
Subscribe to one of our monthly plans to continue reading this article.