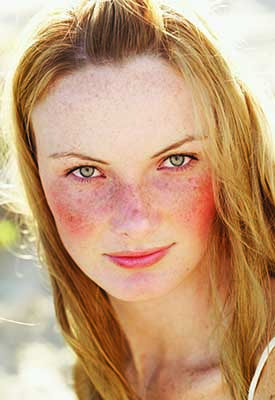 More than one in 20 American adults – approximately 16 million people – suffer from rosacea, but this common skin disease is often misdiagnosed as acne.1 As with acne, there is no simple test to diagnose rosacea. Dermatologists generally identify the condition by observing persistent erythema of the skin in a patient or the emergence of papules or pustules.
More than one in 20 American adults – approximately 16 million people – suffer from rosacea, but this common skin disease is often misdiagnosed as acne.1 As with acne, there is no simple test to diagnose rosacea. Dermatologists generally identify the condition by observing persistent erythema of the skin in a patient or the emergence of papules or pustules.
Unlike acne, people suffering from rosacea are often unaware or confused about the condition. A recent National Rosacea Society (NRS) survey of 1,459 patients2 found that 95 percent knew little or nothing about rosacea’s signs and symptoms prior to their diagnosis and 47 percent said they had never heard of the disease.
This lack of awareness increases the threat rosacea poses because some over-the-counter acne treatments that confused rosacea sufferers might use to treat their condition can actually aggravate it. If left untreated, rosacea tends to become more severe with time and can lead to symptoms like permanent ruddiness of the facial skin, thickening of the skin, and even enlargement of the nose.
New research shows that rosacea’s different symptoms and features may all be part of a continuum of inflammation that may only be detectable histologically and biochemically.3, 4, 5, 6
For these reasons, rosacea’s impact goes beyond the physical. NRS surveys found that more than 90 percent of patients say the condition has lowered their self-confidence and self-esteem, while 41 percent say it has caused them to avoid public contact or cancel social engagements. Among patients with severe symptoms, 88 percent say rosacea has hurt their professional interactions and more than half say it has led them to miss work.7
WHO IS AT RISK?
Fair-skinned adults, especially those with blond hair and blue eyes, are more likely to get rosacea. Particularly susceptible are adults from Celtic or Scandinavian ancestry.8 An NRS survey of 600 rosacea patients found 42 percent were of Irish, German, or English ancestry. The disease can, however, occur in individuals of any race or skin color.
There is also evidence that rosacea may be hereditary.8 NRS research found that 52 percent of rosacea patients had a relative who suffered from the condition.
Age is also a factor. Unlike acne, which typically initially presents in adolescence, 80 percent of cases are diagnosed in people who are at least 30.10
While women are two to three times more likely than men to get rosacea, men tend to experience more severe cases.11 Since the onset of the condition tends to occur in adulthood, rosacea achieves highest prevalence in later years. For example, women experience highest prevalence between the ages of 61 and 65. For men, highest prevalence occurs between the ages of 76 and 80.
One early warning sign of rosacea may be frequent blushing. Some researchers think rosacea occurs when blood vessels expand too easily, causing blushing.12
NEW UNDERSTANDING OF ROSACEA
There has been an abundance of research since 2002, when the initial classification system of rosacea was developed. At that time, the skin disease was thought to fall into four distinct clinical subtypes with apparently different symptoms. In October 2017, a new classification system was published by the NRS’ panel of experts. This new grouping system is based on current understanding of the pathophysiology of rosacea and identifies four major phenotypes and three secondary phenotypes of rosacea, all of which appear to be interrelated.13
MAJOR PHENOTYPES
These major phenotypes may occur independently or concurrently.
Papules and pustules: Dome-shaped, red, acne-like pimples, sometimes accompanied by white heads, often surface in crops across the cheeks and nose. Nodules may also occur.3, 13, 14, 15, 16
Flushing: Frequent and prolonged flushing (sometimes blushing) is common, except in darker skin tones, where flushing may be experienced without obvious erythema. Unlike other erythematous changes, in rosacea, flushing can occur within seconds to minutes in response to neurovascular stimulation by trigger factors.3, 4, 5, 13, 14, 17
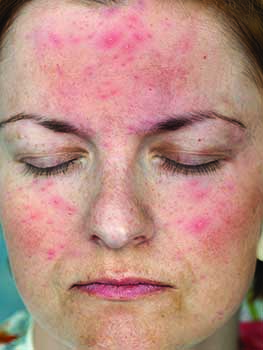 Telangiectasia: Telangiectasias, sometimes known as spider veins, are common signs of rosacea and are predominantly centrofacial. Use of a dermatoscope may allow for detection of telangiectasias in patients with darker skin types.13
Telangiectasia: Telangiectasias, sometimes known as spider veins, are common signs of rosacea and are predominantly centrofacial. Use of a dermatoscope may allow for detection of telangiectasias in patients with darker skin types.13
Ocular manifestations: Ocular rosacea can occur in mild, moderate, or severe cases and may also appear when no other phenotypes are apparent. Signs of ocular rosacea include lid margin telangiectases, interpalpebral conjunctival injection, spade-shaped infiltrates in the cornea, and scleritis and sclerokeratitis. Common symptoms that may suggest ocular rosacea include burning, stinging, light sensitivity, and foreign object sensation.13
SECONDARY PHENOTYPES
Burning or stinging: These sensations may occur, normally on erythematous skin without scales, although scaling may also occur.13,18 Pruritus is not a typical characteristic of rosacea, but may also occur.
Edema: Facial swelling may accompany or follow prolonged erythema or flushing as a result of postcapillary extravasation during inflammation.19 Soft edema may last for days or be aggravated by inflammatory changes. Solid facial edema (persisting hard, nonpitting edema) can occur with rosacea and independently of redness, papules, pustules, or phymatous changes. Commonly, rosacea-related edema involves a combination of blood and lymphatic vessels.3, 13
Dry appearance: Central facial skin may be rough and scaly, resembling dry skin and suggesting an eczematous dermatitis. Rosacea may coexist with seborrheic dermatitis. The dry appearance may be associated with burning or stinging sensations and may be caused by irritation rather than the disease process.13
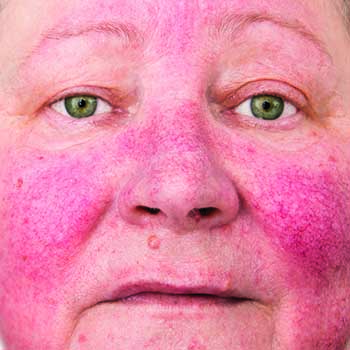
Rosacea’s different phenotypes may appear in different combinations and at different times, but research suggests that all may be manifestations of the same underlying inflammatory continuum3, 4, 5, 6 and that individual cases may progress in severity and worsen to include additional phenotypes.20, 21 The NRS’ panel of experts wrote that, “recent studies point to a multivariate set of pathogenic pathways, including defects in the innate and adaptive immune systems, mast cells and related biochemical mechanisms, and the neurovascular system. It now appears likely that initial erythema and vascular manifestations such as telangiectasia may be in a continuum initiated by a combination of both neurovascular dysregulation and innate immune responses.”13
The phenotype designations are meant to replace the four subtypes widely used clinically to identify the nature of each patient’s rosacea and treat each case. The classical subtypes – vascular, inflammatory, rhinophymatous, and ocular rosacea – are still used clinically by many dermatologists. However, as the NRS panel’s report indicated, they are not accurate diagnostic categories, given the transient and progressive signs and symptoms exhibited by rosacea patients. Earlier research by the NRS had already shown that more than half of rosacea patients suffer from a combination of different subtypes.22 An NRS survey of 1,231 patients found that 72 percent experienced some kind of progression. Overall, 77 percent of patients in the study said they experienced more than one subtype at a time.23
What remains clear is that untreated cases of rosacea generally worsen.
CAUSES
Beyond the apparent genetic connection, the causes of rosacea are not well understood. Researchers believe there is a relationship between triggers of rosacea, flushing reaction, and the permanent swelling of blood vessels close to the skin surface (telangiectasis). Inflammation appears to be linked to the flushing reaction, but it is not clear how. NRS experts have called for additional study.13 Meanwhile, the American Academy of Dermatology reports that researchers are finding important clues about the causes of rosacea:25
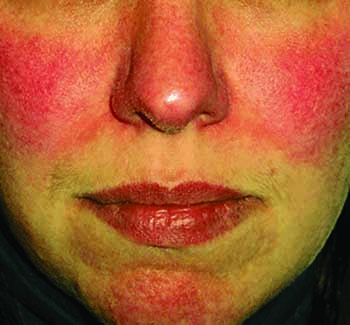 The immune system may play a role. Researchers have found that most people with acne-like rosacea react to a bacterium called bacillus oleronius. The reaction causes their immune systems to trigger an exaggerated inflammatory response. Scientists are not sure this can cause rosacea.
The immune system may play a role. Researchers have found that most people with acne-like rosacea react to a bacterium called bacillus oleronius. The reaction causes their immune systems to trigger an exaggerated inflammatory response. Scientists are not sure this can cause rosacea.
A bug that causes intestinal infections may play a role. This bug, Helicobacter pylori, or H. pylori, is common in people who have rosacea. However, because many people who do not suffer from rosacea may have an H. pylori infection, scientists cannot prove it can cause rosacea.
A mite that lives on everyone’s skin, demodex, may play a role. This mite likes to live on the nose and cheeks, where rosacea often appears. In normal skin, demodex found in small numbers feeds on sebaceous gland contents and is considered part of normal skin microbiome. Studies found that people with rosacea have much larger numbers of demodex mites on their skin. However, some people who do not have rosacea also possess increased facial demodex populations, again indicating it may not cause rosacea, but rather could contribute to abnormal skin physiology characteristic of rosacea.
A protein that protects skin from infection, cathelicidin, may cause the redness and swelling. How the body processes this protein may determine whether a person gets rosacea.
AVAILABLE TREATMENTS ARE NOT CONSISTENT
Rosacea medications provide inconsistent results; and treatment remains aligned with the four clinical subtypes physicians have used to identify and treat the skin disorder since the early 2000s:
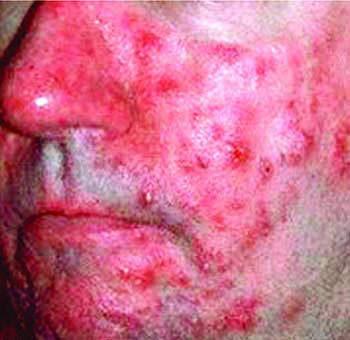
Subtype 1, erythematotelangiectatic (or vascular) rosacea: Primary symptoms include flushing and facial redness. Patients of this traditional subtype tend to be sensitive to topical products and cosmetics; so it is best treated by staying out of the sun or using sunscreen. Recently, the FDA approved two topical agents that constrict superficial capillary blood vessels – 0.33 percent brimonidine gel and 1 percent oxymetazoline cream. Both agents show temporary improvement in facial redness in rosacea.
Subtype 2, papulopustular or inflammatory rosacea: Primary symptoms include persistent redness, papules, or pustules. This subtype has typically been treated with topical or systemic antibiotics or a combination of both. Clinicians usually start with metronidazole cream or gel or topical sulfur/sulfacetamide wash or lotion. Other topical agents found to be effective include azelaic
acid (cream and foam) and ivermectin. Two derivatives of tetracycline, minocycline and doxycycline, are the most common systemic treatments for inflammatory rosacea.
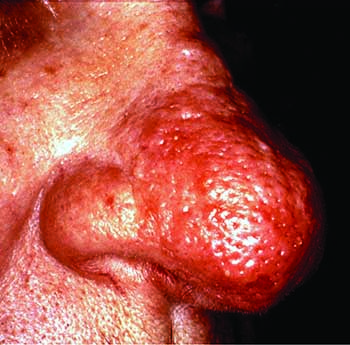
Subtype 3, phymatous rosacea: Primary symptoms include thickening of the skin and excess tissue that enlarges the nose, a condition known as rhinophyma. This severe form of rosacea generally requires more aggressive therapy and systemic antibiotics, sometimes with isotretinoin. Typically, after maximizing the drug regimen, patients are best served by surgical resurfacing of the rosacea-affected area. Electrosurgery can be used to sculpt the rhinophymatous nose, as can use of a laser.
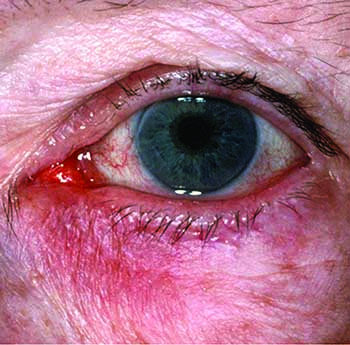
Subtype 4, ocular rosacea: Primary symptoms include eye irritation. Ocular rosacea can only be treated with the use of systemic antibiotics, such as oral tetracycline (250 to 500 milligrams), minocycline (40 to 100 milligrams), or doxycycline (100 milligrams). In some cases, topical corticosteroid eyedrops may help to alleviate symptoms.
Most therapies are associated with adverse side effects. For example, in the case of common topicals, patients often complain of itching, burning, and other discomfort. Rosacea sufferers tend to be especially sensitive to skin irritations. In the case of systemic antibiotics, steady use puts patients at risk of antibiotic resistance and adverse systemic events.
 THE FUTURE
THE FUTURE
Significant research is currently being conducted in rosacea, particularly in papulopustular or inflammatory rosacea, which is, in many ways, a gateway subtype that can lead to more severe cases. Most of the research, 28 of the 43 rosacea studies currently listed on ClinicalTrials.gov, focuses on papulopustular rosacea.
Some of these studies are looking at how medical devices may be useful in treating this subtype, but most are evaluating drugs to supplement or supplant existing treatments, which are not curative and often require patients to try several different medications
and drug combinations to find an effective treatment.27
Many drugs currently used to treat papulopustular rosacea have significant shortcomings. Metronidazole, a cornerstone therapy, has an unknown mechanism of action, but seems to have antimicrobial, antioxidant, and anti-inflammatory properties.28, 29 It is used topically, but is not as effective as some newer agents. Ivermectin, a recent FDA-approved topical agent to treat papulopustular rosacea, is thought to reduce papules by killing demodex mites that live in the sebaceous glands.30, 31, 32 However, adverse effects associated with the topical cream include burning, itching, and dryness at the application site.33
Because of the limitations of current treatments, several companies are researching new twists on existing therapies, such as azelaic acid, an FDA-approved drug found to be effective for papulopustular rosacea.1, 34 Bayer, Novum Pharmaceutical, and Galderma are researching various formulations of azelaic acid and combinations with other therapies. Galderma is trialing Soolantra and Oracea in combination (Ivermectin 1 percent topical cream and doxycycline 40 milligrams in modified release capsules). Cutanea is researching the efficacy of a topical gel formulation of omiganan – a novel, antimicrobial peptide.
Two companies are looking at a new approach to rosacea treatment using different delivery systems for minocycline. BioPharmX is conducting trials with a topical minocycline gel that may provide both the antibiotic and anti-inflammatory benefits of this common tetracycline derivative without the systemic adverse effects associated with oral minocycline. Foamix has been researching a foam formulation of the same antibiotic. These topical products have not been approved by the FDA and are still considered investigational (available only for use in clinical trials).
While oral doxycycline is commonly used to treat rosacea, oral antibiotics are often associated with systemic adverse effects, such as upset stomach, diarrhea, dizziness, photosensitivity, and headaches. In higher doses, doxycycline also has a greater rate of antibiotic resistance than minocycline. The novel topical formulations of minocycline may have the potential to deliver the efficacy of a tetracycline-class drug without the undesireable systemic effects.
Products that are currently in clinical trials may significantly change the way dermatologists treat rosacea in coming years and could potentially reduce adverse effects associated with the treatment.
 References:
References:
1 https://www.rosacea.org/rr/2010/winter/article_1.php
2 https://www.rosacea.org/weblog/rosacea-awareness-month-highlights-warning-signs
3 Schwab VD, Sulk M, Seeliger S, et al. Neurovascular and neuroimmune aspects in the pathophysiology of rosacea. J Invest Dermatol Symp Proc. 2011;15:53-62.
4 Seeliger S, Buddenkotte J, Schmidt-Choudhury A, et al. Pituitary adenylate cyclase activating polypeptide: an important vascular regulator in human skin in vivo. Am J Pathol. 2010;177:2563-2575.
5 Sulk M, Seeliger S, Aubert J, et al. Distribution and expression of non-neuronal transient receptor potential (TRPV) ion channels in rosacea. J Invest Dermatol. 2012;132:1253-1262.
6 Wladis EJ, Iglesias BV, Adam AP, et al. Molecular biologic assessment of cutaneous specimens of ocular rosacea. Ophthal Plast Reconstr Surg. 2012;28:246-250.
7 https://www.rosacea.org/
8 Mikkelsen C, et. al. Rosacea: Time for a new approach. Forum for Nord Derm Ven. (2017) 22:1
9 https://www.rosacea.org/weblog/can_rosacea_be_inherited
10 Spoendlin J, Voegel JJ, Jick SS, Meier CR. A study of the epidemiology of rosacea in the U.K. Br J Dermatol. (2012) Sep;167(3):598-605.
11 Brownlee C. Rosacea. Modern Drug Discovery. (2003) Jan;40.
12 https://www.niams.nih.gov/health-topics/rosacea#tab-causes
13 Gallo RL, Granstein RD, et. al. Standard classification and pathophysiology of rosacea: The 2017 update by the National Rosacea Society Expert Committee. J Am Acad Dermatol. 2017 Oct 28. pii: S0190-9622(17)32297-1.
14 Steinhoff M, Buddenkotte J, Aubert J, et al. Clinical, cellular, and molecular aspects in the pathophysiology of rosacea. J Invest Dermatol Symp Proc. 2011;15:2-11.
15 Trivedi NR, Gilliland KL, Zhao W, et al. Gene array expression profiling in acne lesions reveals marked upregulation of genes involved in inflammation and matrix remodeling. J Invest Dermatol. 2006;126:1071-1079.
16 Buhl T, Sulk M, Nowak P, et al. Molecular and morphological characterization of inflammatory infiltrate in rosacea reveals activation of Th1/Th17 pathways. J Invest Dermatol. 2015;135:2198-2208.
17 Aubdool AA, Brain SD. Neurovascular aspects of skin neurogenic inflammation. J Invest Dermatol Symp Proc. 2011;15:33-39.
18 Lonne-Rahm S-B, Fischer T, Berg M. Stinging and rosacea. Acta Derm Venereol. 1999;79:460-461.
19 Steinhoff M, von Mentzer B, Geppetti P, et al. Tachykinins and their receptors: contributions to physiological control and the mechanisms of disease. Physiol Rev. 2014;94:265-301.
20 Tan J, Blume-Peytavi U, et. al. An observational cross-sectional study of rosacea: clinical associations and progression between subtypes. Br J Dermatol. 2013 Sep;169(3):555-62.
21 Holmes AD, Steinhoff M. Integrative concepts of rosacea pathophysiology, clinical presentation and new therapeutics. Exp Dermatol. 2017;26:659-667.
22 https://rosacea-support.org/wp-content/uploads/2017/05/Rosacea-Time-for-a-New-Approach.pdf
23 https://www.rosacea.org/rr/2004/fall/article_4.php
24 https://www.uspharmacist.com/article/rosacea
25 https://www.aad.org/public/diseases/acne-and-rosacea/rosacea#causes
26 Kligman AM, Christensen MS. Demodex folliculorum: requirements for understanding its role in human skin disease. J Invest Dermatol. 2011 Jan;131(1):8-10.
27 Weinkle AP, Doktor V, Emer J. Update on the management of rosacea. Emer Clin Cosmet Investig Dermatol. 2015;8:159-177. doi: 10.2147/CCID.S58940
28 Feldman SR, Huang WW, Huynh TT. Current drug therapies for rosacea: a chronic vascular and inflammatory skin disease. J Manag Care Spec Pharm. 2014;20(6):623-629.
29 McClellan KJ, Noble S. Topical metronidazole: a review of its use in rosacea. Am J Clin Dermatol. 2000;1(3):191-199. doi: 10.2165/00128071-200001030-00007.
30 Abokwidir M, Fleischer AB. An emerging treatment: topical ivermectin for papulopustular rosacea. J Dermatolog Treat. 2015;26(4):379-380. doi:10.3109/09546634.2014.991672.
31 Brooks M. FDA clears ivermectin cream (Soolantra) for rosacea. Medscape website. medscape.com/viewarticle/837230. Published December 24, 2014. Accessed December 29, 2015
32 Jarmuda S, O’Reilly N, Zaba R, Jakubowicz O, Szkaradkiewicz A, Kavanagh K. Potential role of Demodex mites and bacteria in the induction of rosacea. J Med Microbiol. 2012;61(pt 11):1504-1510. doi: 10.1099/jmm.0.048090-0.
33 Del Rosso JQ. Management of cutaneous rosacea: emphasis on new medical therapies. Exert Opin Parmacother. 2014;15(14):2029-2038. doi: 10.1517/14656566.2014.945423.
34 Johnson AW, Johnson SM. The role of topical brimonidine tartrate gel as a novel therapeutic option for persistent facial erythema associated with rosacea. Dermatol Ther (Heidelb). 2015;5(3):171-181. doi: 10.1007/s13555-015-0078-1.
 Dr. Herron is a physician scientist with nearly three decades of dermatology experience and an active clinical practice in Palo Alto, California. As a member of the Stanford University School of Medicine faculty, he conducted biomedical research, consulted with the biopharmaceutical industry, authored or co-authored more than 30 peer-reviewed papers, and secured several patents in the biomedical field. He serves as medical director for BioPharmX Corporation.
Dr. Herron is a physician scientist with nearly three decades of dermatology experience and an active clinical practice in Palo Alto, California. As a member of the Stanford University School of Medicine faculty, he conducted biomedical research, consulted with the biopharmaceutical industry, authored or co-authored more than 30 peer-reviewed papers, and secured several patents in the biomedical field. He serves as medical director for BioPharmX Corporation.
Want to read more?
Subscribe to one of our monthly plans to continue reading this article.