In this delicate time of personal and physical development, the clinician can create indelible and dramatic changes in not only the health of a teenager’s skin, but also to their self-worth.
 Acne Basics
Acne Basics
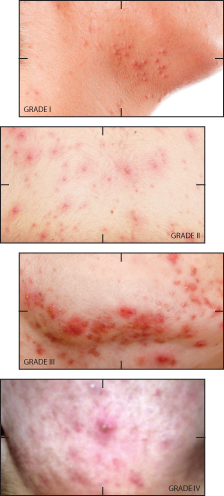
Acne is a skin disease characterized by comedones, papules, pustules, cysts and nodules. The four main drivers of the condition are: increased keratinization within the follicles; increased sebum production; proliferation of Propionibacterium acnes (P. acnes) bacteria; and inflammation. This condition presents in four grades:
Acne simplex
- Grade I may include open or closed comedones. Inflammatory lesions and cysts are not typically seen. Scarring is unlikely in acne simplex as the lesions tend to be superficial; however, patient excoriation (picking) may lead to hyperpigmentation or texture changes. This is a particularly difficult message to get across to teenagers, as they live in the moment and would rather get rid of an obvious blemish, regardless of the long-term consequences.
- Grade II will include the open or closed comedones seen in Grade I, in addition to papules and pustules. Cystic lesions and scarring are not common in acne simplex. Educating the teenager about refraining from picking is also critical with grade II acne.
Acne vulgaris
- Grade III is characterized by inflammation and bacterial lesions. Open and closed comedones may also be seen and scarring will be more common due to the severity of lesions. Prescription therapies prescribed by a physician may be necessary.
- Grade IV presents with deeper cystic and nodular lesions, as well as papules, pustules and comedones. Scarring is very common due to the depth of the lesions. Prescription therapies prescribed by a physician are highly recommended. It is critical that the teenage patient understand the importance of not attempting to extract papules, cysts and nodules. The lesions will not empty, and will potentially rupture the follicle wall below the surface of the skin causing dramatic inflammation, likely scarring and infection.
Acne in adolescents is primarily driven by dramatic shifts in hormones that trigger an increase in sebum production. Additionally, hygiene habits may be lacking or undeveloped, making bacteria and inflammation an issue, especially for teenage boys involved in sports that may not shower after practices. Conversely, some teenage girls may follow marketing and magazines for so-called “miracle cures” and wind up dramatically over-treating their skin, leading to excessive inflammation and dehydration, which only increases the skin’s sebum production. Teenage girls also often attempt to hide their acne with thick, comedogenic foundation and other types of makeup that can dramatically worsen the condition. One of the most important steps for any parent of a tween or teenager that may be suffering from acne is to have a consultation with a dermatologist or licensed skin care professional who can also help to educate the teenage patient on healthy skin practices and determine an appropriate treatment pathway. The severity of the acne can guide what level of care is sought. Lower grades of acne can be addressed by a licensed skin health clinician, while higher grades of more dramatic acne should be seen by a dermatologist.
Puberty
Puberty in girls may begin as early as age 6, but typically begins around 11. Some boys may begin puberty as early as age 9, but 12 is the common onset. Puberty is responsible for triggering the multitude of changes that lead teenagers into physical maturity. During this time of dramatic hormonal shifts and fluctuations, it is quite common for teenagers to experience acne. Although each teenager’s physiology is unique, acne may continue throughout the teenage years, becoming more regulated years later as their hormones begin to balance into appropriate adult levels.
At the o set of puberty, the hormone gonadotropin-releasing hormone (GnRH) is released to exert its effect on the pituitary gland. The pituitary glands of both boys and girls subsequently release two additional hormones into the bloodstream, luteinizing hormone (LH) and follicle-stimulating hormone (FSH).
In teenage males, these hormones trigger the production of testosterone and in female teenagers the production of estrogen is stimulated. This surge in hormones also stimulates an increase in sebum production, which accelerates the development of acne.
Additional Challenge for Girls
As girls enter puberty and begin menstruation, they experience additional cyclical hormone fluctuations that can worsen acne. Even in adult women, monthly acne breakouts can be a common occurrence.
A study published in the Archives of Dermatology asserts that up to 63 percent of women prone to acne also experience cyclical breakouts. Estrogen is the main hormone during the first half of a girl’s menstrual cycle and progesterone asserts dominance in the second half. When progesterone increases, so does sebum production. Occurring concurrently to this progesterone increase is a swelling of the skin and the follicles, which acts to trap this excess sebum, increasing the incidence of acne in the 10 days prior to menstruation.

Effectively Treating Acne in Teenagers
Acne is a hereditary condition, so if either parent suffered from dramatic acne as a teenager, it is likely that their child will as well. It is important for all young children, starting as young as 7 or 8, to learn good skin care habits. The first step in preventing and treating teen acne is to make the daily activity of cleansing, hydrating and treating the skin a regular part of their daily routine. Especially for younger teenagers and tweens, parents typically need to help their child perform the daily cleansing and application of any treatment products and hydrators until they grasp the techniques. These introductory regimens should be uncomplicated and straightforward. Especially at a young age, it should be as simple as gentle cleansing, light hydration at night and a good broad spectrum SPF of at least 30 every day.
Starting with a daily regimen that is complex or hard to follow may make the teenager decide it is more trouble than it is worth. Clearly, not keeping the skin clean and balanced is a recipe for a worsening of breakouts. Once a child is older and the acne condition is potentially worsened, the gentle cleansers should be substituted with benzoyl peroxide washes, salicylic acid treatment products, topical retinoids, bacteria-fighting hydrators and non-oily broad spectrum SPF products.
Regardless of the age of the teenager, all four main causes of acne must be addressed in their daily care regimen – even in a few simple steps. The products used must control sebum production, while also reducing follicular and surface hyperkeratinization, P. acnes proliferation and inflammation.
 Controlling Sebum
Controlling Sebum
Although controlling sebum production in acne-prone skin is a critical component in the improvement of the condition, it is also imperative to understand that over-drying a patient’s skin, even if they are oily, will cause the skin to compensate by producing an excessive amount of sebum. This will cause additional breakouts, rather than improving the condition.
With their typically narrow worldview, teenagers can often migrate to aggressive, bracing astringents and overly drying spot treatments thinking that they can kill-off the acne. This practice is highly counter-productive and will not only dehydrate the skin, but will also cause inflammation and aggravate the acne. Use of gentle astringents that also moisturize will avoid this over-production of sebum. Additionally, studies have indicated that acneic skin is deficient in essential fatty acids (EFA). In the absence of the EFA, the skin instead produces excess sebum. Although many regimens for acne taut their oil-free formulations, using hydrators that contain EFA-rich beneficial oils like borage seed oil, grape seed oil and wheat germ oil, will actually help to reduce sebum production and alleviate breakouts.
Reducing Hyperkeratinization
One of the initial triggers in the development of acne papules is the increased adherence of keratinocytes to the follicle wall in combination with increased sebum production, resulting in a plugged pore. Skin cells oftentimes do not desquamate properly on their own, creating a buildup of surface cells that result in trapped oil and bacteria. This then leads to the follicle becoming a de-oxygenated environment, a perfect stage for the proliferation of anaerobic P. acnes bacteria. A safe and effective way to reduce surface and follicular hyperkeratinization is the use of gentle, blended peeling solutions applied in a professional setting on a bi-weekly basis. These treatments control bacteria and oil production, as well as loosen the impacted stratum corneum, stimulate improved desquamation and promote effective penetration of topically applied remedies. At home, teenage patients can use gentle exfoliant products and clay-type masks to absorb oil, detoxify the skin and remove the excess cell debris that contributes to impaction. Topical retinoids are also useful for this purpose.
The term “retinoids” encompasses the family of vitamin A derivatives. They help to increase cellular proliferation and turnover, bringing healthy cells to the surface more quickly. Although every teenager’s skin has a differing level of sensitivity, prescription strength retinoids can cause surface irritation in many skin types and may be worse for the young patient. Although prescription strengths may be a necessary treatment for more severe grades of acne, pure retinol may be a better option for younger teenagers. Retinol is a gentle vitamin A derivative that is converted to retinoic acid in the skin. It is effective, yet non-irritating. Using a daily care product with low-level pure retinol in conjunction with regular, gentle professional peels is an excellent standard of care.
 Minimizing P. Acnes
Minimizing P. Acnes
One of the critical steps in clearing acne is controlling the P. acnes bacteria that drive the condition. Use of topical antibacterial and antimicrobial agents, and oral or topical antibiotics (when applicable) are acceptable ways to control the bacteria population. Topical oxygen sources, such as benzoyl peroxide and hydrogen peroxide, reduce the anaerobic bacteria’s ability to thrive and proliferate.
Treatments performed by licensed skin health professionals that increase circulation and blood flow will deliver oxygen, which will lead to a decrease in P. acnes and assist in the clearing of active lesions. Light massage during application of products will also increase circulation, although it should be avoided in grades III and IV acne, as it could lead to cross-contamination. Facial massage is an excellent way to introduce the teenage patient to the concept of facial treatments. Many are initially uncomfortable with the idea of someone touching their skin, especially if they carry shame about their acne condition. Gentle massage not only stimulates circulation, but it induces a relaxed state that can be beneficial to any teenager. The act of touch can also help build the trust relationship
between clinician and teenager, increasing the level of compliance to which they will commit in order to achieve their goal of a clear complexion.
Products containing benzoyl peroxide (BPO) are available up to 10 percent over-the-counter (OTC) and at higher percentages by prescription only. Because BPO exerts its effect quickly, it is a good choice for washes. It is also effective in lotions and creams to penetrate pores to eliminate current blemishes and prevent future lesions. Unlike other ingredients like salicylic acid, it is not necessary for the BPO to remain on the skin for any extended period of time for it to be effective. Daily use of BPO products will increase sun sensitivity, so daily SPF use is critical. The inflammation caused by unprotected sun exposure is highly detrimental to the acneic teenager, so if you truly do not believe they will be compliant with sunscreen, it is best to forgo BPO in favor of ingredients that do not increase sun sensitivity.
 Fighting Inflammation
Fighting Inflammation
Inflammation is both a cause and result of acne. When the population of P. acnes increases, sebum is broken down into irritating free fatty acids, stimulating an immune response. White blood cells weaken the follicular wall, which can result in follicular rupture and increased inflammation. Employing anti-inflammatory topical ingredients soothes and prevents irritation and inflammation. Aloe vera, salicylic acid, bisabolol, panthenol, licorice extract, boldine extract, resveratrol and EGCG from green tea are just some of the extremely effective ingredients available to control inflammation.
Additionally, ultraviolet exposure is a known cause of inflammation in the skin. Many teenagers have the misconception that sun exposure will “dry up” their acne. In fact, the inflammation that results from UV exposure will undoubtedly worsen their condition. There are now broad spectrum SPF products designed especially for breakout-prone and acneic skin that are light and leave no residue or emollience on the skin. This is a critical part of every healthy skin regimen, but is particularly integral for anyone using products and ingredients that increase sun sensitivity, like BPO and retinoids.
Acne patients who use topical agents that address all four of these drivers simultaneously will help to reduce excess sebum and increase the cell turnover rate of their skin. Combined with gentle exfoliation, they will ensure that P. acnes and excess cell debris will not be trapped within follicles in a deoxygenated environment and allowed to progress into a worsened acne condition.
 Professional Treatment Choices for Teenagers: Start Slowly
Professional Treatment Choices for Teenagers: Start Slowly
Although the etiology of acne is essentially the same regardless of the age of the patient, things like youth, inexperience and emotional immaturity can make the application of more active professional treatments unwise in young teenage patients. Once they are initiated into the world of professional skin care, many teenagers can easily tolerate gentle blended chemical peels. Until you feel the patient has a comfort level with the process, it is best to instead use proteolytic enzyme treatments, low-level alpha hydroxy acid (AHA) and beta hydroxy acid (BHA) blends, and mask treatments. There are many professional products available today that incorporate therapeutic levels of ingredients like salicylic acid, but combine it with calming anti-inflammatory agents to make the treatment experience more pleasant and less frightening for a tween or teenager than a straight acid peel.
When treating acne it is best to set appointments two weeks apart. This is enough time to not create too much inflammation in the skin, but close enough together to not allow bacteria and surface impaction to escalate and lead to an increase in lesions.
Another critical piece to engaging in the professional treatment of a teenager’s skin is the relationship you build with the patient and their parent. Calling them at home the day following treatment and again several days later will help allay any fears they may have and will allow you to intervene if they are experiencing any complications, but were unwilling to reach out for help.
Caring for More Than Just a Teenager’s Skin
The teenage years are fraught with not only raging hormones, changing bodies and potential acne, but are also the time in life where each child is trying to shape themselves as people, understand the world, get their hearts broken, try to fit in – and the list goes on. To head into this time of emotional fragility and uncertainty feeling ashamed of the way their skin looks can leave scars on their self-esteem as well as their skin. Many clinicians have stories of the teenagers they have helped. The boy that did not feel like he could show his face at school or the girl too ashamed of her skin to attend the prom, and even teenagers whose acne has made them feel that life may not be worth living. It may sound dramatic, but their world revolves on the “here and now” at their age. Often something that we as adults can see will pass seems completely insurmountable for a teenager. Be aware of the signs that their emotions need care, in addition to their skin. Also, be mindful of when it may be wise to suggest outside counseling assistance to a teenager’s parent. Sometimes an effective acne treatment pathway for a teenager involves not just caring for their skin.
Treating the teenage acne patient requires more than just an understanding of the disease, and the most efficient and effective ways to eradicate the condition. Being cognizant of the myriad changes and challenges with the unique stage of development that encompasses the teenage years will help the clinician to successfully treat not only a teenager’s acne, but build their sense of self-worth as well. Being able to have a positive impact on the life of a teenager is a wonderful and affirming part of our work as skin health professionals.
 As a board-certified dermatologist, pediatrician and fellowship-trained pediatric dermatologist practicing out of Scottsdale, Arizona, Cynthia Price, M.D. is dedicated to providing excellent, innovative and compassionate patient care. She specializes in adult, pediatric, surgical and cosmetic dermatology. Price is a fellow of the American Academy of Dermatology and the American Academy of Pediatrics, as well as a member of the American Society for Dermatologic Surgery, the Society for Pediatric Dermatology, the Women’s Dermatology Society, the Phoenix Dermatology Society and the American Medical Association.
As a board-certified dermatologist, pediatrician and fellowship-trained pediatric dermatologist practicing out of Scottsdale, Arizona, Cynthia Price, M.D. is dedicated to providing excellent, innovative and compassionate patient care. She specializes in adult, pediatric, surgical and cosmetic dermatology. Price is a fellow of the American Academy of Dermatology and the American Academy of Pediatrics, as well as a member of the American Society for Dermatologic Surgery, the Society for Pediatric Dermatology, the Women’s Dermatology Society, the Phoenix Dermatology Society and the American Medical Association.
