Skin conditions can be distressing at a visible level, however they are often triggered by responses occurring inside the body. Skin, being the largest organ of the body, can represent what is taking place from internal stress, to hormonal fluctuations, to an unhealthy lifestyle. The most common skin conditions seen by aestheticians are acne, rosacea and hyperpigmentation. Although there are actions we can take to assist clients in reducing the appearance of these unappealing conditions, treatments are not always skin deep. Aside from the physical effects of skin conditions, there are emotional obstacles that can develop as well.
 The job of the skin care professional is not only to treat the outer appearance, but to also help the client build confidence. Inopportunely, the most common skin conditions are the most difficult to control, resulting in possible reoccurrence over a lifetime.
The job of the skin care professional is not only to treat the outer appearance, but to also help the client build confidence. Inopportunely, the most common skin conditions are the most difficult to control, resulting in possible reoccurrence over a lifetime.
Acne
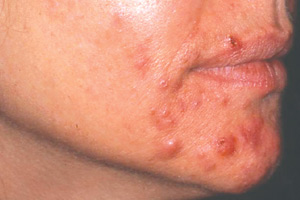
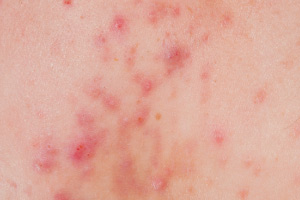
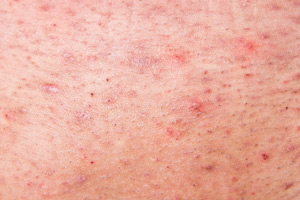
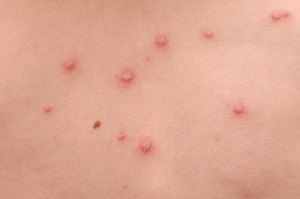
A chronic condition, acne affects virtually everyone at some point in their lives. Although it is commonly seen in teenagers, many adults experience bouts of acne as well. Hormonal fluctuation, stress, illness, poor health and certain medications can all have an indirect effect on acne formation. People who suffer from acne can become severely depressed due to poor self-esteem. Depression is a horrible disease that is hidden by many; it can have debilitating effects including lethargy, loss of appetite, physical weakness, behavioral problems, and even feelings of hopelessness leading to suicidal thoughts or actions. Unfortunately, acne is most common during the teenage years – a time when self-image plays a crucial role in emotional development. It is of the utmost importance that the skin care professional is extra sensitive to the client’s feelings and concerns during this time. Skin care professionals should take more time to consult with the client on what has and has not worked, while offering reassurance that they will work together to get the symptoms under control.
 Acne can be broken up into four grades. Grade I, the mildest form of acne, consists of blackheads and whiteheads. This type of acne is often treated successfully with topical products and aesthetic treatments. Grade II acne commonly has a large presence of comedones along with occasional papules and pustules. Grade III acne consists of inflamed papules and pustules along with blackheads and whiteheads. Grade IV acne is a severe form of acne in which the person affected will likely have a combination of blackheads, whiteheads, papules, pustules and nodules or cysts. It is often accompanied by severe inflammation that may become very red and even purplish.
Acne can be broken up into four grades. Grade I, the mildest form of acne, consists of blackheads and whiteheads. This type of acne is often treated successfully with topical products and aesthetic treatments. Grade II acne commonly has a large presence of comedones along with occasional papules and pustules. Grade III acne consists of inflamed papules and pustules along with blackheads and whiteheads. Grade IV acne is a severe form of acne in which the person affected will likely have a combination of blackheads, whiteheads, papules, pustules and nodules or cysts. It is often accompanied by severe inflammation that may become very red and even purplish.
Those with Grades III and IV acne should be seen by a physician for their recommended course of treatment. Medical providers may prescribe topical or internal medications, as well as provide in-office procedures. Antibiotics are typically the first choice made by physicians to reduce P. acnes bacteria.
Lasers alone, or lasers used in combination with a topically applied solution known as photodynamic therapy (PDT), are highly successful, in-office medical treatments for acne. PDT is a combination of a topically applied photo-sensitizing drug and laser or light therapy, including blue light LED. These light therapies work by activating a protein that is released by the bacteria P. acnes to become a killer protein. The protein then destroys the bacteria and the surrounding inflamed acne cells. Injury is limited to only the acne lesions and normal skin is not affected.
 Hyperpigmentation
Hyperpigmentation
Another condition that can cause emotional distress is hyperpigmentation. There are an estimated six million women living in the United States with melasma.1 There are some that try to hide the condition by tanning, which triggers pigmentation and can be frustrating to the client. It can also take a lot of time, resources and work to get visible symptoms under control, only for the slightest trigger to cause reoccurrence. Aestheticians must take extra precaution when dealing with hyperpigmented areas of the skin. Any suspicious lesions should be checked by a medical professional before a treatment is administered. Although aestheticians can never diagnose, it is important to refer the client to a physician for any questionable marks on the skin.
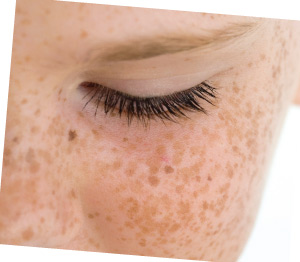
Sun-induced pigment typically has a freckled appearance and is distributed throughout the skin. This pigment can show up in all skin types, although it is more commonly seen in Fitzpatrick Types I to III. Ultraviolet exposure from the sun, tanning beds and fluorescent lights stimulate an increase of melanin production to protect skin cells from further damage. Actinic keratosis are scaly pigmented lesions caused by a cumulative effect of ultraviolet damage. These lesions are considered pre-cancerous and should be treated by a physician to reduce the risk of further invading the skin.
Melasma, also known as chloasma or the pregnancy mask, is a tan or deep brown facial skin discoloration typically shown in the center of the face. It is most prevalent in the cheeks, forehead and upper lip. Melasma typically shows up as dense areas of pigment with defined borders, as opposed to sun-induced pigmentation which is more sporadic across the face in a freckle pattern. Although it can affect anyone, melasma is particularly common in women; pregnant women who are taking oral contraceptives or on hormone replacement therapy are most commonly affected. Melasma may be a long-lasting, recurring condition that is easily stimulated by inflammation, especially sun exposure. Melasma may go away after pregnancy or with the discontinued use of hormone therapy. In severe cases of melasma, the pigment is deposited in the dermis, making it very difficult to treat. 
 Treatments for hyperpigmentation often include products with skin lightening ingredients, lasers and/or chemical peels. Hydroquinone and other pigment lightening agents including kojic acid, azelaic acid, emblica and licorice root work on varying pathways of the melanogensis process to reduce pigment. Topical retinoids are used in conjunction to increase cellular turnover and balance the distribution of melanin. Topical products are used in conjunction to increase cellular turnover and balance the distribution of melanin. Topical products work best when paired with in-office treatments to enhance results.
Treatments for hyperpigmentation often include products with skin lightening ingredients, lasers and/or chemical peels. Hydroquinone and other pigment lightening agents including kojic acid, azelaic acid, emblica and licorice root work on varying pathways of the melanogensis process to reduce pigment. Topical retinoids are used in conjunction to increase cellular turnover and balance the distribution of melanin. Topical products are used in conjunction to increase cellular turnover and balance the distribution of melanin. Topical products work best when paired with in-office treatments to enhance results.
Chemical peels work well on many cases of hyperpigmentation, however care must be taken on darker skin types. Several levels of peels are available from very superficial, commonly offered by aestheticians, to very deep, provided by physicians. Physicians commonly use visible light lasers, IPL or ablative lasers to treat sun-induced and post-inflammatory pigmentation. There are queries related to the amount of inflammation that these treatments may cause, therefore they are usually not the first choice of treatment for those with melasma. Furthermore, protecting the skin from further damage with antioxidants and sunscreens is vital to maintaining results.
Rosacea
Most often associated with people of Celtic or Scandinavian ancestry, rosacea is a persistent disorder of the skin characterized by vascular dilation of the central face, including the nose, cheeks and chin. Primary symptoms include redness and flushing of the face, along with the presence of telangiectasias (small, dilated blood vessels near the surface of the skin). The severity of these symptoms vary from person to person. Women between the ages of 30 and 60 are most commonly affected by rosacea. Clinical features are characterized by periods of exacerbation and remission. Rosacea has also been shown to have negative effects on emotional health as well. A survey conducted by The National Rosacea Society showed nearly 70 percent of rosacea sufferers stating that rosacea had lowered their self-esteem and self-confidence, many reporting embarrassment, anxiety and even depression.2 The primary focus should be on actively educating the client on how common rosacea is and how to avoid triggers in order to control symptoms.
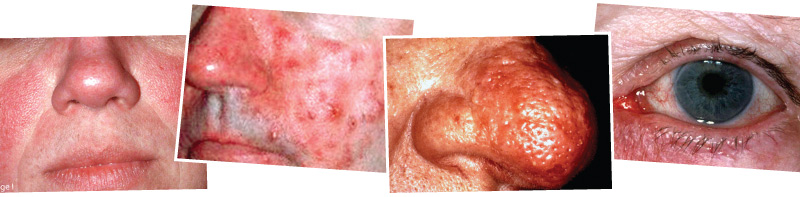
The source of rosacea is unknown, but there are many theories as to what causes this condition. There are four stages of rosacea. Depending on the stage of rosacea, the spectrum of clinical findings vary widely. Stage I, also known as erythematotelangiectatic rosacea, is characterized by erythema and flushing. Telangiectasias may also be present in Stage I, though they are not always. Stage II rosacea, or papulopustular rosacea, is often referred to as acne rosacea. Redness and flushing is commonly present along with papules and pustules. There is usually stinging and burning involved, making anti-inflammatory agents a must for this condition. Stage III, or phymatous rosacea, is more common in men than women, presenting with thickening of the skin. This most often occurs on the nose and is known as rhinophyma. This irregular surface may also show up on the chin, forehead and cheeks. There will also be a presence of pronounced redness and telangiectasias. Stage IV, or ocular rosacea, includes the presence of red, watery, swollen eyes along with other characteristics shown in other stages. The patient usually experiences burning, stinging and even blurred vision in the eyes.
 As there is currently no cure for rosacea, treatment is based on symptom management. This includes lifestyle changes, such as reducing sun exposure, eliminating spicy food and alcohol from diets, controlling stress, and using non-irritating skin care products. Additionally, the use of steam, hot towels and vigorous massage should be avoided. Product recommendations should include gentle cleansers, anti-inflammatory agents, and the use of a zinc oxide-based sunscreen. Avoiding triggers of rosacea and home care can help to alleviate symptoms, however in-office treatments will enhance results.
As there is currently no cure for rosacea, treatment is based on symptom management. This includes lifestyle changes, such as reducing sun exposure, eliminating spicy food and alcohol from diets, controlling stress, and using non-irritating skin care products. Additionally, the use of steam, hot towels and vigorous massage should be avoided. Product recommendations should include gentle cleansers, anti-inflammatory agents, and the use of a zinc oxide-based sunscreen. Avoiding triggers of rosacea and home care can help to alleviate symptoms, however in-office treatments will enhance results.
 Severe cases of rosacea and those with inflammation should only be treated by a physician. Topical or oral antibiotics may be prescribed to relieve the inflammatory lesions associated with rosacea. Metronidazole is another topical prescription commonly used to fight bacteria associated with rosacea. Other topical agents that have been used with varying amounts of success include azelaic acid, sulfacetamide, clindamycin, erythromycin and benzoyl peroxide. These agents should be used for at least four to six weeks before assessing the results.
Severe cases of rosacea and those with inflammation should only be treated by a physician. Topical or oral antibiotics may be prescribed to relieve the inflammatory lesions associated with rosacea. Metronidazole is another topical prescription commonly used to fight bacteria associated with rosacea. Other topical agents that have been used with varying amounts of success include azelaic acid, sulfacetamide, clindamycin, erythromycin and benzoyl peroxide. These agents should be used for at least four to six weeks before assessing the results.
Visible light lasers and light therapy have been used by medical professionals with positive results in decreasing vascular lesions associated with rosacea in Stages I and II. Rhinophyma or other areas of thickened skin associated with Stage III rosacea can be treated with dermabrasion or ablative lasers. Dermabrasion is a treatment using a wire brush or diamond wheel to remove excess skin whereas ablative lasers remove the outer layers of skin using heat. Although these medical treatments show great results, conditions may return.
Taking this all into consideration, it is important to note that clients with all of these skin conditions can benefit from learning camouflage makeup techniques which can facilitate emotional well-being and confidence. Leading a healthy lifestyle can also have positive effects on a client’s emotional well-being and self-perception. As Dr. Barakin and Dr. DeKoven discuses in their article “Psychosocial Effect of Common Skin Diseases,” it is pertinent that skin care professionals remind their clients of the interplay between skin disease and stress. They should also address the importance of reducing stress with such techniques as deep breathing or meditation, yoga, and writing a journal.3 These recurring skin conditions cause emotional distress; therefore it is important that we show an understanding of the client’s fears and doubts in order to initiate their emotional recovery. Kind words and a gentle touch are simple methods of reassurance that can be very effective for easing the client’s stress level.
 There is definitely more than meets the eye in several skin conditions. The priority of aestheticians and other cosmetic providers is to make clients feel better about themselves. Skin care professionals should provide information on what may be happening between the skin, as well as all available options for treatment. Persistent conditions should always be seen by a physician to ensure safe and effective results.
There is definitely more than meets the eye in several skin conditions. The priority of aestheticians and other cosmetic providers is to make clients feel better about themselves. Skin care professionals should provide information on what may be happening between the skin, as well as all available options for treatment. Persistent conditions should always be seen by a physician to ensure safe and effective results.
References
1Alai, Nili N., M.D., F.A.A.D. “Melasma Symptoms, Signs, Causes, Diagnosis, Treatment, Prevention and Prognosis by MedicineNet.com.” MedicineNet. N.p., n.d. Web. 10 June 2013. http://www.medicinenet.com/melasma/article.htm>.
2”National Rosacea Society Improving 16 Million Lives through Awareness, Education and Research.” Rosacea.org. N.p., n.d. Web. 10 June 2013. http://www.rosacea.org/>.
3Barankin, Benjamin, M.D., and Joel DeKoven, M.D. “Psychosocial Effect of Common Skin Diseases.” Canaidan Family Physician 48 (2002): 712-16. Web. 10 June 2013. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2214020/pdf/12046366.pdf>.
 Terri Wojak has been an aesthetician for over 16 years. As the aesthetics director, business manager and lead educator of True U Esthetics, Wojak lectures at multiple aesthetic conferences each year and is frequently published in industry magazines. She has trained over 1,000 aestheticians and medical professionals in the art of advanced skin care with a specialization in techniques used in a cosmetic medical setting. Beyond the techniques and treatments, Wojak makes sure students are trained to succeed in whatever setting they choose, with extensive experience and knowledge in business development and marketing. She has unmatched passion and drive for increasing knowledge of skin care in cosmetic medicine, her compelling personality and love for aesthetics makes Wojak one of the most sought out experts and educators in the industry.
Terri Wojak has been an aesthetician for over 16 years. As the aesthetics director, business manager and lead educator of True U Esthetics, Wojak lectures at multiple aesthetic conferences each year and is frequently published in industry magazines. She has trained over 1,000 aestheticians and medical professionals in the art of advanced skin care with a specialization in techniques used in a cosmetic medical setting. Beyond the techniques and treatments, Wojak makes sure students are trained to succeed in whatever setting they choose, with extensive experience and knowledge in business development and marketing. She has unmatched passion and drive for increasing knowledge of skin care in cosmetic medicine, her compelling personality and love for aesthetics makes Wojak one of the most sought out experts and educators in the industry.
Want to read more?
Subscribe to one of our monthly plans to continue reading this article.